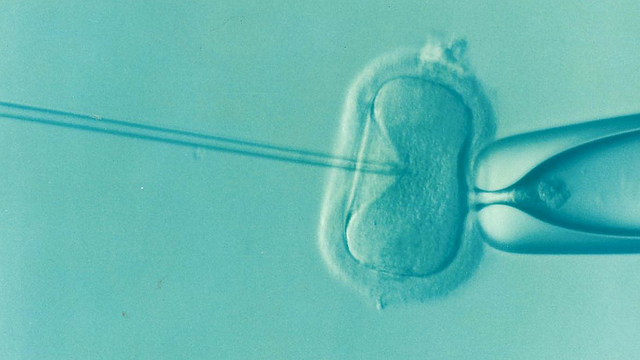
Comprehensive Guide to Azoospermia Treatment and ICSI Options in Pakistan
Get a free topical map and start building content authority today.
azoospermia treatment in Pakistan requires a clear diagnostic pathway, access to sperm retrieval methods, and careful planning for ICSI (intracytoplasmic sperm injection). This guide explains common causes, the available surgical and laboratory techniques used in Pakistan, and practical steps for patients and clinicians to improve chances of success.
Detected intent: Informational
- Start with semen analysis and hormonal/genetic tests to distinguish obstructive vs non-obstructive azoospermia.
- Sperm retrieval options include PESA/TESA (percutaneous) and TESE/micro-TESE (surgical); ICSI is the standard fertilization method with retrieved sperm.
- Use the 5-point Azoospermia Assessment Checklist for clinic evaluation. Consider costs, lab quality, and surgeon experience when choosing care in Pakistan.
Azoospermia treatment in Pakistan: overview and why diagnosis matters
Azoospermia means no sperm in the ejaculate and is categorized as obstructive azoospermia (OA) or non-obstructive azoospermia (NOA). Correct classification guides treatment choices: OA often responds well to surgical sperm retrieval or reconstruction, while NOA may require micro-TESE and has lower retrieval rates. Accurate diagnosis reduces unnecessary procedures and helps patients plan for assisted reproductive technology (ART) such as ICSI for azoospermia.
How diagnosis is performed
Semen analysis and repeat testing
At least two high-quality semen analyses separated by 2–4 weeks are needed to confirm azoospermia. Laboratory standards should follow guidelines from reproductive medicine societies to avoid false negatives.
Hormonal and genetic testing
Measure serum FSH, LH, testosterone, and prolactin. Elevated FSH commonly suggests testicular failure (NOA). Genetic tests include karyotype and Y-chromosome microdeletion screening; these influence prognosis and counseling. Refer to authoritative guidance such as the World Health Organization (WHO) for semen analysis standards and infertility definitions: WHO infertility fact sheet.
Sperm retrieval techniques and ICSI for azoospermia
Obstructive azoospermia options
Techniques commonly used in Pakistan for OA include:
- PESA (percutaneous epididymal sperm aspiration) — minimally invasive, used when obstruction is in the epididymis.
- TESA (testicular sperm aspiration) — needle aspiration from the testis, quick and low-cost.
- Surgical reconstruction — vasovasostomy or vasoepididymostomy when a surgical correction is feasible and desired.
Non-obstructive azoospermia and micro-TESE
Micro-TESE (microsurgical testicular sperm extraction) is the preferred approach for NOA because it allows targeted sampling of seminiferous tubules under an operating microscope. Retrieval rates vary by cause and preoperative markers (e.g., FSH, testicular volume).
ICSI for azoospermia
ICSI is the fertilization method of choice when using surgically retrieved sperm. Even immotile or few sperm can be used for injection into oocytes. Embryology lab expertise and good culture conditions strongly influence embryonic development and implantation.
5-point Azoospermia Assessment Checklist (named framework)
Use the following checklist before proceeding to invasive procedures or ICSI:
- Confirm azoospermia with repeat semen analyses and review lab standards.
- Complete hormonal panel (FSH, LH, testosterone) and relevant imaging (scrotal ultrasound).
- Perform genetic screening when indicated (karyotype, Y-chromosome microdeletion).
- Discuss sperm retrieval options (PESA/TESA/TESE/micro-TESE) and expected retrieval probabilities.
- Evaluate ART laboratory quality, ICSI experience, and counseling about success rates and costs.
Practical tips for patients and clinicians in Pakistan
- Choose clinics with documented embryology lab quality and experienced microsurgeons—ask about micro-TESE cases and success statistics.
- Request copies of semen analysis reports and any genetic testing; these records reduce repeat testing and guide management.
- Consider freezing any retrieved sperm if feasible—cryopreservation avoids repeated retrieval procedures.
- Get a second opinion if initial evaluations recommend immediate donor options without clear diagnostic workup.
Costs, availability, and realistic outcomes
Costs vary widely across Pakistan. Less invasive procedures like PESA/TESA are generally less expensive than micro-TESE and ICSI combined. Success depends on female partner factors, embryology lab quality, and whether viable sperm were retrieved. For NOA, retrieval rates are lower; counseling and expectations management are essential.
Common mistakes and trade-offs
Common mistakes
- Skipping genetic tests that could alter counseling or reveal inherited conditions.
- Proceeding to ICSI without confirming sperm viability or without cryopreservation backup.
- Choosing clinics based only on price rather than lab accreditation, surgeon experience, or concrete outcome data.
Trade-offs
Less invasive retrieval (PESA/TESA) trades off lower invasiveness for potentially lower retrieval success in NOA. Micro-TESE increases retrieval chances but requires specialized surgical skill and longer operative time. Deciding between immediate reconstruction (for OA) vs. sperm retrieval plus ICSI involves weighing time, success probability, cost, and patient preference.
Real-world example
Scenario: A 34-year-old male with two semen analyses showing azoospermia and an elevated FSH of 22 mIU/mL. Scrotal ultrasound shows normal testicular size. Genetic testing shows no Y-chromosome microdeletion. The fertility team recommended micro-TESE with possible ICSI. Micro-TESE retrieved a small number of viable sperm that were cryopreserved, and a subsequent ICSI cycle produced one high-quality embryo and a successful pregnancy. This scenario highlights the importance of hormonal testing, genetic screening, targeted retrieval, and embryo lab quality.
Core cluster questions for internal linking and further articles
- How do micro-TESE and conventional TESE compare for non-obstructive azoospermia?
- What genetic tests are recommended before sperm retrieval for azoospermia?
- How should couples prepare financially and emotionally for ICSI after sperm retrieval?
- What are the indicators that obstructive azoospermia can be treated with reconstruction instead of retrieval?
- How does cryopreservation of surgically retrieved sperm affect ICSI timing and outcomes?
Choosing a clinic in Pakistan: quick evaluation checklist
- Verify embryology lab accreditation and ask about ICSI success rates and live-birth rates.
- Confirm surgeon experience with micro-TESE and request case volumes when possible.
- Check availability of genetic counseling and comprehensive diagnostics on-site.
- Ask about sperm cryopreservation facilities and backup plans for failed retrievals.
Next steps and when to seek referral
Refer patients to a urologist with reproductive microsurgery expertise or to a reproductive endocrinologist if initial tests are inconclusive. Multidisciplinary teams improve decision-making for azoospermia management and ICSI planning.
Resources and standards
Follow internationally recognized standards for semen analysis and infertility counseling. The World Health Organization (WHO) provides guidance on laboratory methods and infertility definitions; consult official resources for up-to-date testing standards and patient counseling frameworks.
FAQ
What is azoospermia treatment in Pakistan and what steps are involved?
Treatment begins with repeat semen analyses and hormonal/genetic testing to classify OA vs NOA. Options include sperm retrieval (PESA, TESA, TESE, micro-TESE), possible surgical reconstruction for OA, and ICSI when sperm are retrieved. Clinic choice, lab quality, and counseling are essential steps.
Can ICSI for azoospermia use sperm retrieved from micro-TESE?
Yes. ICSI is routinely used with sperm obtained by micro-TESE when sperm counts are very low or sperm are non-motile. Embryology lab experience is important for handling and selecting viable sperm.
What genetic tests should be done before sperm retrieval?
Common tests include karyotype and Y-chromosome microdeletion screening. These tests influence prognosis and reproductive counseling, and may be recommended based on FSH levels, testicular volume, or family history.
How should patients evaluate success rates and costs for sperm retrieval and ICSI?
Request clinic-specific success data (ideally live-birth rates), ask about lab accreditation, surgeon experience, and include cryopreservation costs. Compare trade-offs between procedure types and expected retrieval probabilities.
How long does recovery take after micro-TESE or TESA?
Recovery from TESA/PESA is usually short (a few days). Micro-TESE recovery may involve more discomfort and a longer recovery window (1–2 weeks) due to the surgical approach; follow post-op instructions and activity restrictions provided by the surgical team.