Realistic Hair Transplant Expectations: Timeline, Recovery, and What to Expect
Get a free topical map and start building content authority today.
Detected intent: Informational
Understanding realistic hair transplant expectations is the first step toward a successful outcome: it sets the timeline, reduces anxiety, and helps align goals with clinical reality. This guide explains what to expect before, during, and after surgery, with a named checklist, a short case scenario, and practical tips to manage recovery and results.
- Most visible improvement occurs between 6–12 months; full maturation can take up to 18 months.
- Expect temporary shedding (shock loss), visible scabs, and staged growth phases.
- Follow a clear recovery plan, use the EXPECT Checklist, and manage expectations with the surgeon’s photos and measurements.
Realistic hair transplant expectations: what actually happens
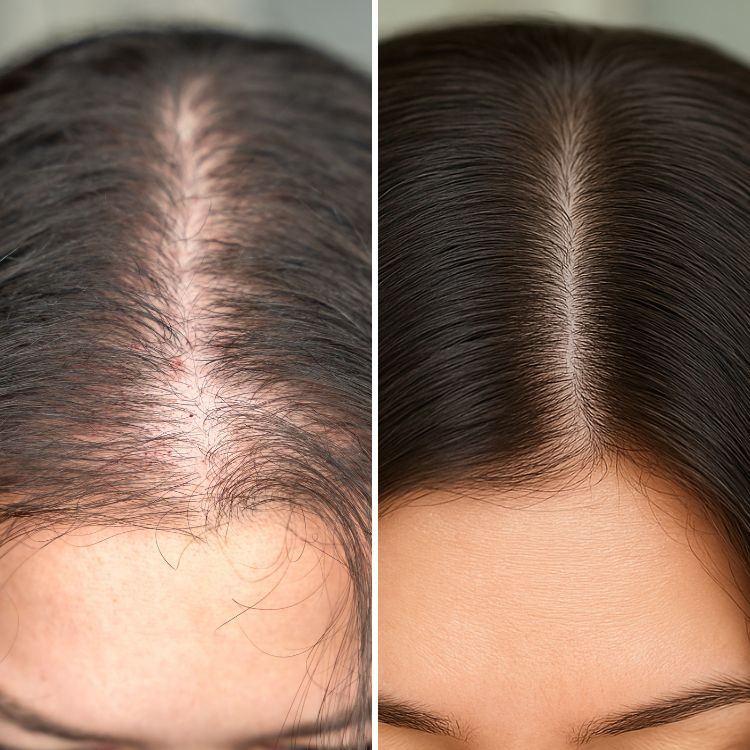
A hair transplant moves grafts from a donor area to a recipient site; realistic hair transplant expectations include an initial healing phase, temporary shedding of transplanted hairs, and a gradual regrowth cycle. Results depend on technique (FUE vs FUT), graft count, donor density, individual healing, and post-op care. Use measurements and photos from the clinic to set measurable goals rather than relying on anecdotes.
EXPECT Checklist — a named framework to prepare and measure progress
The EXPECT Checklist is a practical framework to align expectations and action:
- Evaluate goals: Document desired density and areas to cover with photos and measurements.
- Xplain procedure details: Confirm technique, graft estimate, and risks with the surgeon.
- Plan recovery: Arrange time off, sleeping setup, medications, and follow-up visits.
- Educate on timeline: Note likely shedding, early regrowth, and final maturation windows.
- Communicate milestones: Take standardized photos at 1 week, 1 month, 3 months, 6 months, 12 months.
- Tackle complications early: Know signs of infection, poor graft take, or abnormal scarring and contact the clinic.
Typical hair transplant recovery timeline
Immediate (Days 0–14)
Sutures or micro-puncture healing, scabs, mild swelling, and tenderness are common. Follow wash instructions and avoid strenuous activity. Most scabs fall off by day 10–14.
Short-term (Weeks 2–12)
Transplanted hairs often shed between weeks 2–8 ("shock loss"). This is normal. The scalp continues to heal; numbness that persists for weeks is common.
Medium-term (3–6 months)
Early regrowth begins around 3 months for many patients; density increases gradually through month 6. This is a good time to assess whether adjunct treatments (PRP, topical therapies) are needed.
Long-term (6–18 months)
Most patients see substantial visual improvement by 9–12 months; full maturation and texture changes can take up to 18 months. Expect further subtle thickening and naturalization during this period.
Real-world scenario
Case: A 38-year-old male had a 2,200-graft FUE procedure to restore a receding hairline. First two weeks: scabbing and mild swelling, returned to work after 10 days. Weeks 3–8: shock loss of transplanted hairs. Month 4: fine vellus regrowth. Month 8: 60–70% visible density improved. Month 12: full cosmetic result with matured hair shafts and natural hairline blending.
Practical tips to manage expectations and recovery
- Take standardized photos (same lighting and angle) at every milestone from the EXPECT Checklist.
- Follow the clinic’s wash and sleeping guidelines for the first 10–14 days to protect grafts.
- Plan work and social life around the early visible healing phase; scabs and redness are normal.
- Track progress by percentage improvement rather than daily appearance—small changes add up over months.
- Ask for objective measures: graft count, donor density, and follicular units per centimeter squared when setting goals.
Trade-offs and common mistakes
Trade-offs
Higher graft counts can improve density but increase recovery burden and risk of donor site thinning. FUE has smaller scars but may require more sessions than FUT for the same density. Combining treatments (PRP, minoxidil) can accelerate visual results but adds cost and complexity.
Common mistakes
- Expecting immediate final results—early appearance is misleading.
- Relying solely on before-and-after photos without measurable data like graft count or standardized photos.
- Ignoring post-op instructions (sleeping position, sun protection, activity limits), which can reduce graft survival.
Core cluster questions
- How long is the typical hair transplant recovery timeline?
- What causes shock loss after a hair transplant?
- How to measure and document hair transplant progress?
- When should one consider a second session or touch-up?
- Which post-op behaviors most affect graft survival?
Safety, standards, and where to verify facts
For evidence-based patient information and safety recommendations, review guidance from national health resources; for example, the NHS provides an overview of indications, risks, and aftercare for hair transplant procedures (NHS: Hair transplants). Clinics should follow established consent and infection-control standards.
FAQ
What are realistic hair transplant expectations?
Realistic expectations include temporary shedding, progressive regrowth starting around 3 months, noticeable improvement at 6–9 months, and full maturation by 12–18 months. Final density depends on donor supply and the planned graft count.
How long is the hair transplant recovery timeline?
Early healing takes 1–2 weeks, shock loss occurs in weeks 2–8, regrowth often begins near month 3, and significant cosmetic results typically appear between 6–12 months.
When will my transplant look natural?
Many patients reach a natural appearance between 9–12 months; texture and thickness can continue to improve up to 18 months.
Can anything speed up visible results?
Adjuncts like topical minoxidil, low-level laser therapy, or PRP may support growth but do not replace realistic timelines. Discuss benefits and evidence with the clinic.
What signs require contacting the clinic?
Persistent or spreading redness, severe pain, pus drainage, fever, or sudden, unexplained loss of grafts beyond the typical shock loss window should prompt immediate clinic contact.