Weight Loss Injections Explained: Safety, Effectiveness, Options, and Next Steps
Get a free topical map and start building content authority today.
Weight loss injections have become an increasingly discussed option for medical weight management, combining prescription medications with lifestyle support. This guide explains what weight loss injections are, how they work, who they may suit, and the safety and monitoring needed before choosing this path.
Weight loss injections (primary keyword: weight loss injections) typically refer to prescription injectable medications that reduce appetite, slow gastric emptying, or change metabolic signals. They can produce clinically meaningful weight loss when combined with diet and activity changes but require medical evaluation for safety and monitoring. Detected intent: Informational.
Weight Loss Injections: What they are and how they work
Weight loss injections are prescription medications administered by subcutaneous injection that act on hormones and receptors involved in appetite, satiety, and glucose regulation. Common mechanisms include GLP-1 receptor agonism, which increases fullness and reduces caloric intake, and other peptide-based pathways that influence metabolism. These medications are part of a broader medical approach—not a standalone solution—and are typically prescribed after a clinical assessment.
Key mechanisms and related terms
- GLP-1 receptor agonists (glucagon-like peptide-1): promote satiety and slow gastric emptying.
- Appetite suppression and energy-balance modulation.
- Adjunctive therapy combined with diet, physical activity, and behavioral support.
Who regulates and provides guidance?
Regulatory oversight and safety guidance come from national agencies and medical societies. For reliable information about obesity and treatment approaches, consult public health resources from official organizations such as the Centers for Disease Control and Prevention (CDC).
Types of injections, categories, and common examples
Options are organized by mechanism and approval status. Examples are included for illustration, not endorsement.
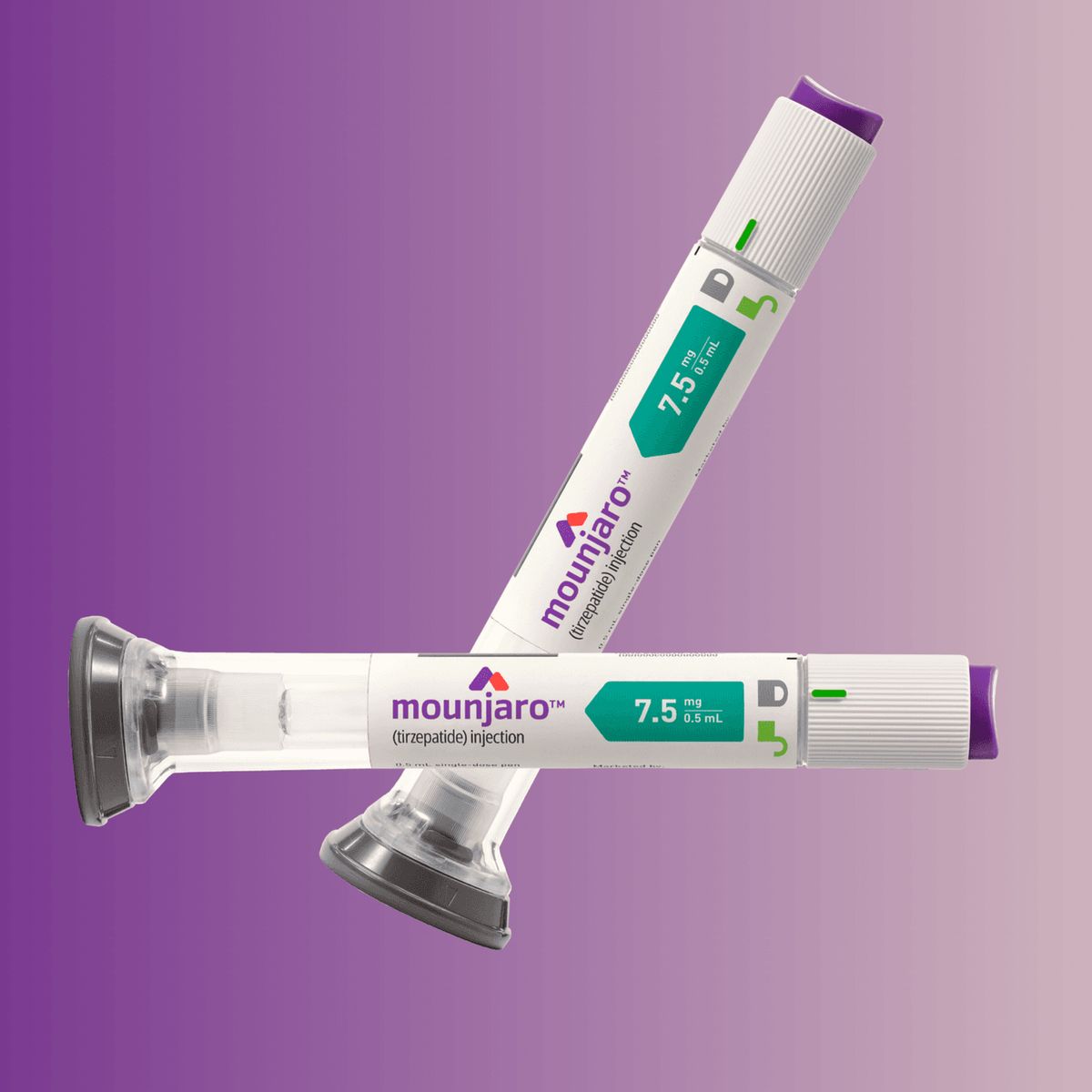
- GLP-1 receptor agonists: often used for diabetes and, at certain doses, for weight management. (Example: semaglutide—mentioned as a drug class example.)
- Other peptide-based or hormone-targeting injections: under research or used off-label in some clinical contexts.
- Closely supervised combination protocols: injections plus structured dietary and behavioral programs offered by medical clinics.
Secondary keywords in context
Search terms that commonly appear in patient queries include GLP-1 weight loss injections and semaglutide injection for weight loss; those terms point to the same category of mechanism but can differ by dose, labeling, and indicated use.
SCALE Injection Readiness Framework: a practical checklist
A concise, named framework helps evaluate readiness and fit. Use the SCALE checklist before considering injections:
- Screening: medical history, BMI, metabolic labs, and contraindications.
- Clinical goals: realistic target weight loss and functional objectives.
- Alternatives reviewed: lifestyle-first plans, behavioral therapy, and surgical options where appropriate.
- Labs & monitoring plan: baseline labs (liver, kidney, glucose) and regular follow-up schedule.
- Education & consent: understanding side effects, injection technique, and cost/coverage.
Safety checklist
- Confirm prescription by a licensed clinician and documented follow-up plan.
- Check for pregnancy, pancreatitis history, or other contraindications.
- Arrange baseline labs and a plan for dose adjustments or discontinuation.
Real-world example: a typical clinical scenario
A 42-year-old patient with BMI 34 and prediabetes discusses weight management with a primary care clinician. After lifestyle counseling and a nutrition plan, medication options are reviewed. A GLP-1 receptor agonist is started at a low dose with a plan for dose escalation, regular check-ins every 3 months, and glucose monitoring. Side effects such as nausea are expected initially; the care team adjusts timing and provides dietary tips to reduce symptoms. After six months, the patient achieves a meaningful decrease in weight and improves HbA1c; the ongoing plan emphasizes continued lifestyle work alongside medication monitoring.
Practical tips for anyone exploring injections
- Confirm a clear diagnosis and documented clinical goal before starting therapy; medications should support, not replace, lifestyle changes.
- Ask the prescribing clinician for a monitoring schedule and emergency contacts for severe side effects.
- Learn proper injection technique with a trained clinician or nurse to reduce irritation and dosing errors.
- Verify insurance coverage or out-of-pocket cost estimates up front and ask about patient assistance programs if cost is a barrier.
Trade-offs and common mistakes
Trade-offs to consider
- Effectiveness vs. cost: some medications produce larger average weight loss but can be expensive or require prior authorization.
- Symptom relief vs. long-term commitment: stopping medication often leads to partial regain unless behavioral changes are sustained.
- Rapid results vs. side effects: faster titration can increase gastrointestinal symptoms; slower titration improves tolerability.
Common mistakes
- Starting injections without a documented plan for follow-up and lab monitoring.
- Expecting medication alone to solve lifestyle-related contributors to weight.
- Using unverified online sources or non-prescription products; only prescribed medications from licensed providers are safe and legal.
Core cluster questions for related coverage
- How do GLP-1 weight loss injections differ from oral weight-loss medications?
- What monitoring is required during injectable weight-loss therapy?
- Which patients are good candidates for prescription weight management injections?
- How should side effects of injectable weight loss medications be managed?
- What are the long-term outcomes and maintenance strategies after stopping injections?
FAQ
Are weight loss injections safe and effective?
Clinical trials and regulatory reviews show that some injectable medications can produce clinically meaningful weight loss for many people when combined with lifestyle changes. Safety depends on individual medical history, dose, and monitoring. A licensed clinician should assess risks and benefits before use.
How quickly do results appear with GLP-1 weight loss injections?
Some weight and appetite changes may appear within weeks, but meaningful, sustained loss usually occurs over months with dose titration and continued lifestyle support. Rapid early changes vary by individual.
What side effects should be expected and when should medical help be sought?
Common side effects include nausea, constipation, or mild gastrointestinal upset during dose escalation. Seek immediate medical attention for severe abdominal pain, signs of allergic reaction, or unexpected rapid heart rate or breathing difficulty.
Can injections be used with other weight-loss treatments?
Combination therapy is sometimes appropriate, but interactions and cumulative risks must be reviewed by a clinician. Surgical options or other medications require coordinated care and specialist input.
How long is treatment usually continued?
Duration varies by goals and response. Some people use medication long-term as part of chronic disease management; others may taper or stop after achieving goals under medical supervision. Long-term planning should include strategies for maintaining results.
For evidence-based public health information and clinical guidance on obesity and treatment strategies, consult recognized health authorities such as the CDC: CDC - Obesity.