PRP for Skin Rejuvenation: How Platelet-Rich Plasma Works, Benefits, Risks, and a Practical Checklist
Get a free topical map and start building content authority today.
What Is PRP (Platelet-Rich Plasma) and Why Use PRP for Skin Rejuvenation?
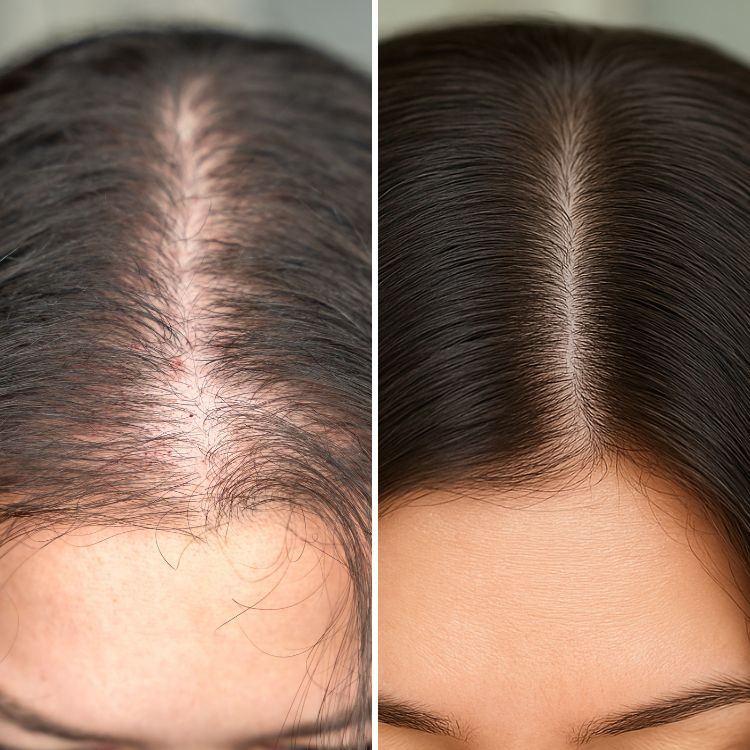
PRP for skin rejuvenation uses a concentrated portion of a patient’s own blood—platelet-rich plasma—to support skin repair and stimulate collagen production. The term platelet-rich plasma (PRP) describes blood plasma with a higher-than-normal platelet concentration, which contains growth factors and signaling proteins that can promote tissue healing. This guide explains how PRP works, who is a reasonable candidate, safety considerations, and how to plan practical treatments.
Detected intent: Informational
How PRP Works: Biology, Preparation, and Delivery
PRP preparation begins with venipuncture to collect a small volume of blood. A centrifuge separates red blood cells from plasma and platelets, yielding a platelet-rich layer. Platelets release growth factors—such as platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), and vascular endothelial growth factor (VEGF)—that modulate inflammation, encourage collagen synthesis, and recruit repair cells. Delivery methods include:
- Injection into targeted areas (e.g., nasolabial folds, under-eye hollows)
- Microneedling combined with PRP to increase absorption and stimulate dermal remodeling
- Superficial topical application after controlled epidermal abrasion
Benefits, Evidence, and Who Sees Results
PRP for skin rejuvenation may improve fine lines, skin tone, and texture and can speed healing after resurfacing treatments. Evidence ranges from clinical trials to observational dermatologic studies; consistent outcomes often depend on technique, platelet concentration, and patient factors such as age, skin condition, and lifestyle. Typical expectations:
- Noticeable but modest improvement after 1–3 sessions; optimal results often need 3 treatments spaced 4–6 weeks apart
- Enhanced results when PRP is combined with microneedling or laser resurfacing
- Gradual collagen remodeling continuing for months after treatment
PRP Safety & Effectiveness Checklist (named framework)
- Confirm candidacy: assess skin type, medical history, anticoagulant use, and active infection.
- Verify practitioner credentials: board-certified dermatologist or plastic surgeon with PRP experience.
- Confirm sterile protocol: single-use needles, sterile centrifuge tubes, and clean handling.
- Check platelet concentration: aim for a clinically appropriate enrichment (practitioner should document protocol).
- Plan follow-up: schedule 4–6 week follow-up and full treatment series if needed.
Procedure Walk-Through: What to Expect
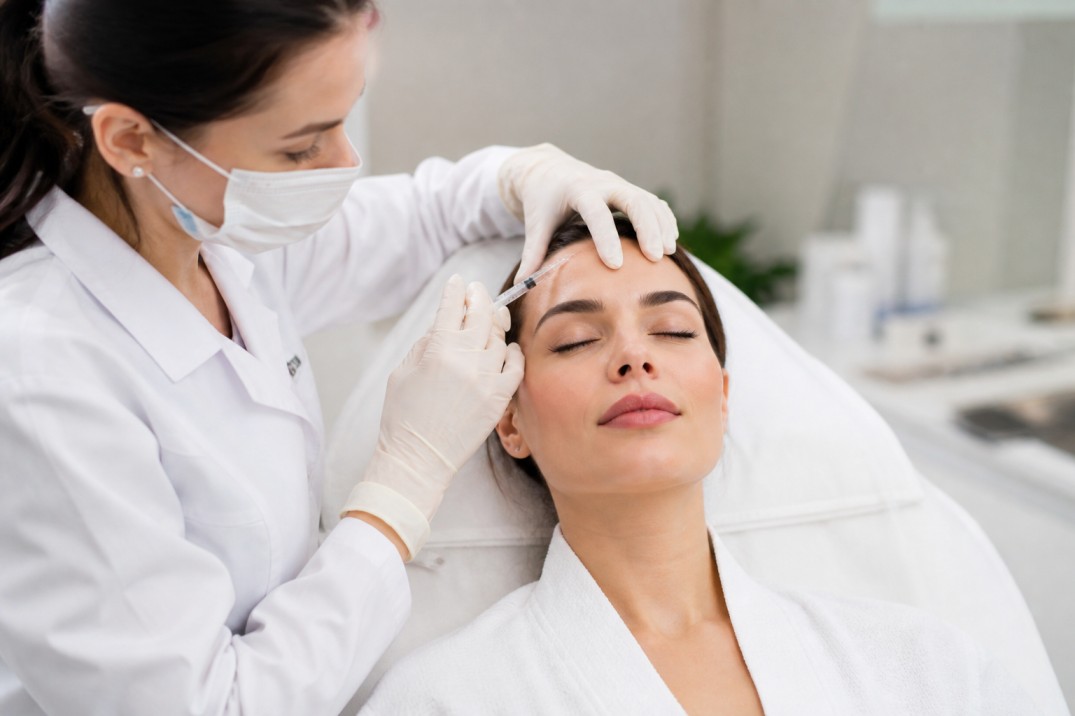
Typical in-office flow: brief medical intake and photos; blood draw; centrifugation (10–15 minutes); local anesthetic or topical numbing if injecting; application or injections of PRP; brief recovery period. Most patients leave the office within an hour.
Real-world Example: A Typical Patient Scenario
Case: A 42-year-old with early sun damage and mild nasolabial folds seeks skin texture improvement. After medical clearance, three microneedling+PRP sessions were scheduled at 6-week intervals. Mild swelling and redness lasted 48–72 hours after each session. By 3 months after the final treatment, the patient reported smoother texture and improved glow; fine lines were reduced but not eliminated. Maintenance treatments were advised annually.
Practical Tips for Better Outcomes
- Stop blood-thinning supplements (aspirin, high-dose fish oil) only with clinician guidance at least 5–7 days before the procedure.
- Avoid smoking in the weeks around treatment—smoking impairs microcirculation and healing.
- Follow a post-procedure skincare plan: gentle cleanser, broad-spectrum sunscreen, and avoid aggressive exfoliation for 1–2 weeks.
- Expect a series of treatments; track results with standardized photos taken before and after each session.
Trade-offs and Common Mistakes
Trade-offs
PRP is autologous (uses the patient’s own blood) which reduces allergic risk, but it is operator-dependent—results depend heavily on technique and platelet concentration protocols. Combining PRP with other resurfacing modalities often increases effectiveness but also raises cost and recovery time.
Common mistakes
- Assuming a single session will provide dramatic changes—most improvements are incremental.
- Skipping sterile technique or using non-medical settings increases infection risk and poor outcomes.
- Choosing providers without documented experience in PRP protocols and technique.
Recovery, Risks, and When to Seek Care
Recovery is usually short: mild swelling, bruising, and redness for 1–7 days. Less common risks include infection, prolonged swelling, and nodules from improper injection depth. Contact a qualified clinician if fever, increasing pain, pus, or spreading redness occurs. For regulatory guidance and to confirm provider credentials, consult a professional dermatology organization such as the American Academy of Dermatology (AAD).
Core cluster questions (useful for internal linking and related content)
- How many PRP treatments are needed for facial rejuvenation?
- What are the differences between PRP and stem cell therapies for skin?
- How does PRP combined with microneedling compare to microneedling alone?
- What are the contraindications for PRP cosmetic treatments?
- How long do PRP facial results typically last?
Practical pre-treatment checklist
Before scheduling: confirm medical history, stop advised supplements, hydrate, and arrange a short downtime window for recovery. Ask the clinic to document their PRP protocol and expected costs up front.
Costs and Access
PRP is typically an elective cosmetic service; costs vary widely by region, provider, and combination treatments. Insurance generally does not cover cosmetic PRP procedures.
Evidence and Professional Guidance
Clinical studies and dermatology reviews report variable but generally positive outcomes for texture and mild wrinkle reduction; systematic reviews note heterogeneity in study designs and the need for standardized protocols. Consulting certified dermatology or plastic surgery societies is recommended for best-practice standards.
Frequently asked questions
What is PRP for skin rejuvenation and how quickly does it work?
PRP for skin rejuvenation uses concentrated platelets from the patient’s blood to stimulate collagen and tissue repair. Noticeable changes typically appear over several weeks to months, with full remodeling often taking 3–6 months after a treatment series.
Is PRP safe for all skin types?
PRP itself is autologous and low-risk, but safety depends on delivery method and the practitioner’s experience. People with active infections, certain blood disorders, or on anticoagulant therapy may not be candidates.
Does PRP hurt and what is the recovery time?
Sensation varies by delivery method; topical numbing and local anesthetic reduce discomfort for injections. Typical recovery is 24–72 hours for redness and swelling, though bruising can last longer.
How many sessions of PRP are typically recommended?
Most protocols recommend a series of 2–4 treatments spaced 4–6 weeks apart, followed by maintenance sessions as needed. Results and schedules should be personalized by a treating clinician.
Can PRP be combined with microneedling or laser treatments?
Yes. PRP is commonly combined with microneedling or laser resurfacing to enhance healing and boost collagen stimulation, but combination therapies increase cost and can extend recovery, so technique and timing should be managed by an experienced provider.