Advanced Knee Pain Treatment in Singapore: Faster Recovery Strategies
The phrase advanced knee pain treatment Singapore describes modern clinical approaches available in the city-state to reduce pain, restore mobility, and speed healing after injury or degenerative change. This guide explains diagnostic steps, non-surgical and surgical options, rehabilitation strategies, and a practical RECOVER checklist for faster recovery.
- Early diagnosis—imaging and specialist assessment—shapes the right treatment plan.
- Non-surgical options (physiotherapy, targeted injections, orthobiologics) often produce fast gains; surgery is reserved for structural damage or failed conservative care.
- Rehabilitation, activity modification, and a coordinated care plan accelerate return to function.
- Use the RECOVER checklist to track readiness, compliance, and expected timelines.
Detected intent: Informational
Advanced knee pain treatment Singapore: how care is evaluated and selected
Why accurate diagnosis matters
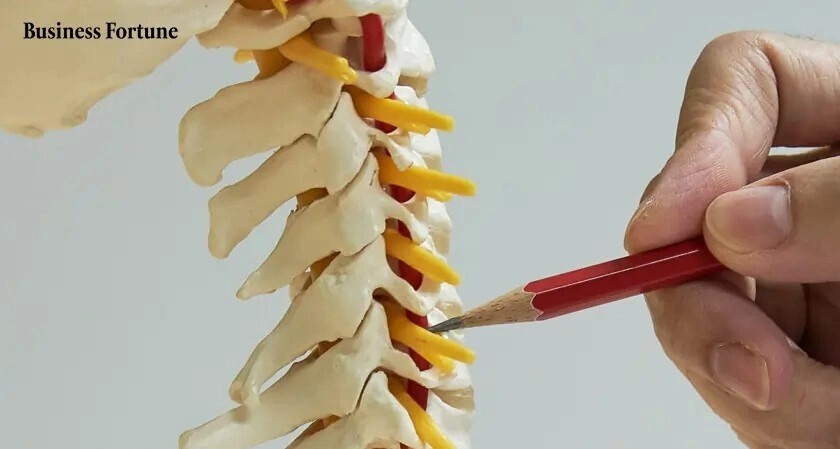
Knee pain arises from many sources: ligament injury, meniscal tears, cartilage degeneration (osteoarthritis), patellofemoral pain, bursitis, or referred pain from the hip or spine. Accurate diagnosis via clinical history, physical tests, and imaging (X‑ray, MRI, ultrasound) targets treatment to the root cause and prevents unnecessary or ineffective interventions. Local standards and hospital guidelines follow the Ministry of Health framework for referral and subspecialty involvement, helping ensure consistent pathways for care (Ministry of Health Singapore).
Initial assessment components
- History: onset, mechanism, daily impact, prior treatments.
- Exam: alignment, ligament stability, joint line tenderness, range of motion.
- Imaging: weight-bearing X‑ray for alignment; MRI for soft-tissue detail; diagnostic ultrasound for guided injections.
- Functional tests: gait, squat, single-leg balance to assess load tolerance.
Evidence-based treatment options and timelines
Non-surgical care (first line for most cases)
Non-surgical knee pain treatments include targeted physiotherapy, progressive strengthening, activity modification, bracing or taping, and pain-management strategies. For faster recovery, structured rehabilitation programs that combine manual therapy, progressive loading, and neuromuscular retraining are most effective. The secondary keyword non-surgical knee pain treatments Singapore applies to many patients seeking to avoid surgery.
Injections and orthobiologics
Therapeutic injections—corticosteroid for short-term inflammation control, hyaluronic acid for symptomatic relief in degenerative joints, or orthobiologics (platelet-rich plasma, cell-based therapies)—are adjuncts when conservative measures slow progress. Response varies by diagnosis and patient factors; set realistic expectations about the timeline and magnitude of improvement.
Surgical options and when to consider them
Surgery is appropriate for repairable structural damage (e.g., unstable meniscal tears, ACL rupture) or when conservative care fails for advanced osteoarthritis. Typical procedures include arthroscopic repair, ligament reconstruction, osteotomy to correct alignment, and partial or total knee arthroplasty. Accelerated recovery protocols, including multimodal analgesia and early mobilization, can shorten hospital stays and speed function restoration.
Rehabilitation strategy and the RECOVER checklist
Recovery is a staged process. The RECOVER checklist is a simple framework to standardize planning and monitor progress during rehabilitation:
- R — Readiness: confirmed diagnosis, cleared medically for activity
- E — Education: patient understands goals, restrictions, and milestones
- C — Conditioning: graded strengthening and mobility program
- O — Optimization: pain control, swelling management, sleep and nutrition
- V — Volume progression: controlled load increases with objective metrics
- E — Evaluation: regular outcome measures (pain scores, function tests)
- R — Return criteria: objective benchmarks for work/sport return
Typical recovery timelines
- Minor sprains/tendinopathy: 2–8 weeks with focused rehab.
- Meniscal repair or moderate surgery: 8–16 weeks for routine activities; 4–6 months for higher-demand return.
- Ligament reconstruction or arthroplasty: 6–12 months depending on goals and rehabilitation adherence.
Real-world example: accelerated, conservative recovery scenario
A 52-year-old recreational runner in Singapore presents with medial knee pain and MRI-confirmed early medial compartment osteoarthritis plus mild varus alignment. A coordinated plan uses: a 12-week physiotherapy program emphasizing hip and quadriceps strengthening, activity modification away from high-impact running to cycling and controlled strengthening, a single guided hyaluronic injection for symptomatic relief, and a home-based progressive loading log. After eight weeks the patient reports 60% pain reduction and resumed low-impact exercise; surgical options deferred pending ongoing improvement.
Practical tips to speed recovery
- Follow a structured exercise program tailored to the diagnosis; avoid random or excessive loading that increases inflammation.
- Use objective measures (timed single-leg squat, 30-second sit-to-stand) to track progress rather than pain alone.
- Manage swelling proactively (compression, elevation, short-term ice) to enable earlier mobility work.
- Coordinate care—physio, orthopedics, and primary care—to align medication, lab oversight, and return-to-activity milestones.
- Prioritize sleep, protein intake, and smoking cessation—these systemic factors influence tissue healing rate.
Trade-offs and common mistakes when pursuing faster recovery
Trade-offs to consider
- Speed versus durability: aggressive timelines and early return to sport may increase re-injury risk if tissue strength is incomplete.
- Injections trade immediate symptom relief for variable long-term benefit; repeated corticosteroids can weaken tissue.
- Surgery can restore structure but carries recovery time, perioperative risk, and the need for prolonged rehab.
Common mistakes
- Skipping proper imaging or specialist input for persistent or atypical pain.
- Progressing activity based on enthusiasm rather than objective readiness markers.
- Relying solely on passive treatments without a progressive loading program.
Core cluster questions
- How long does non-surgical knee pain treatment typically take to show results?
- What are the risks and benefits of knee injections versus physiotherapy?
- When is surgery recommended for meniscal tears or ACL injuries?
- How should rehabilitation be structured after partial knee replacement?
- What objective tests indicate readiness to return to sport after knee injury?
Frequently asked questions
What are the most effective advanced knee pain treatment Singapore options for faster recovery?
Effective approaches combine accurate diagnosis, structured physiotherapy, targeted injections when indicated, and timely surgical intervention for structural problems. A multidisciplinary plan with progressive loading and measurable milestones tends to produce the fastest, most sustainable recovery.
Can physiotherapy alone fix chronic knee pain?
Physiotherapy often reduces pain and improves function for many chronic knee conditions, especially when the program is individualized and progressive. Persistent structural pathology or failed conservative care may still require procedural or surgical options.
Are injections like platelet-rich plasma widely used in Singapore?
Orthobiologic injections are available and sometimes used for degenerative knee conditions. Evidence quality varies by modality and condition; discuss expected benefits, costs, and alternative strategies with a clinician.
How soon after knee surgery can rehabilitation begin?
Rehabilitation typically begins within 24–48 hours after many arthroscopic procedures and on the first postoperative day for joint replacements under enhanced recovery protocols. Early mobilization reduces complications and supports faster functional gains.
Is imaging always necessary for knee pain?
Not always. Plain X‑rays are useful for suspected osteoarthritis or alignment issues; MRI is indicated when soft-tissue injury or an unexplained mechanical symptom is suspected. Clinical judgment determines imaging need to avoid unnecessary tests.