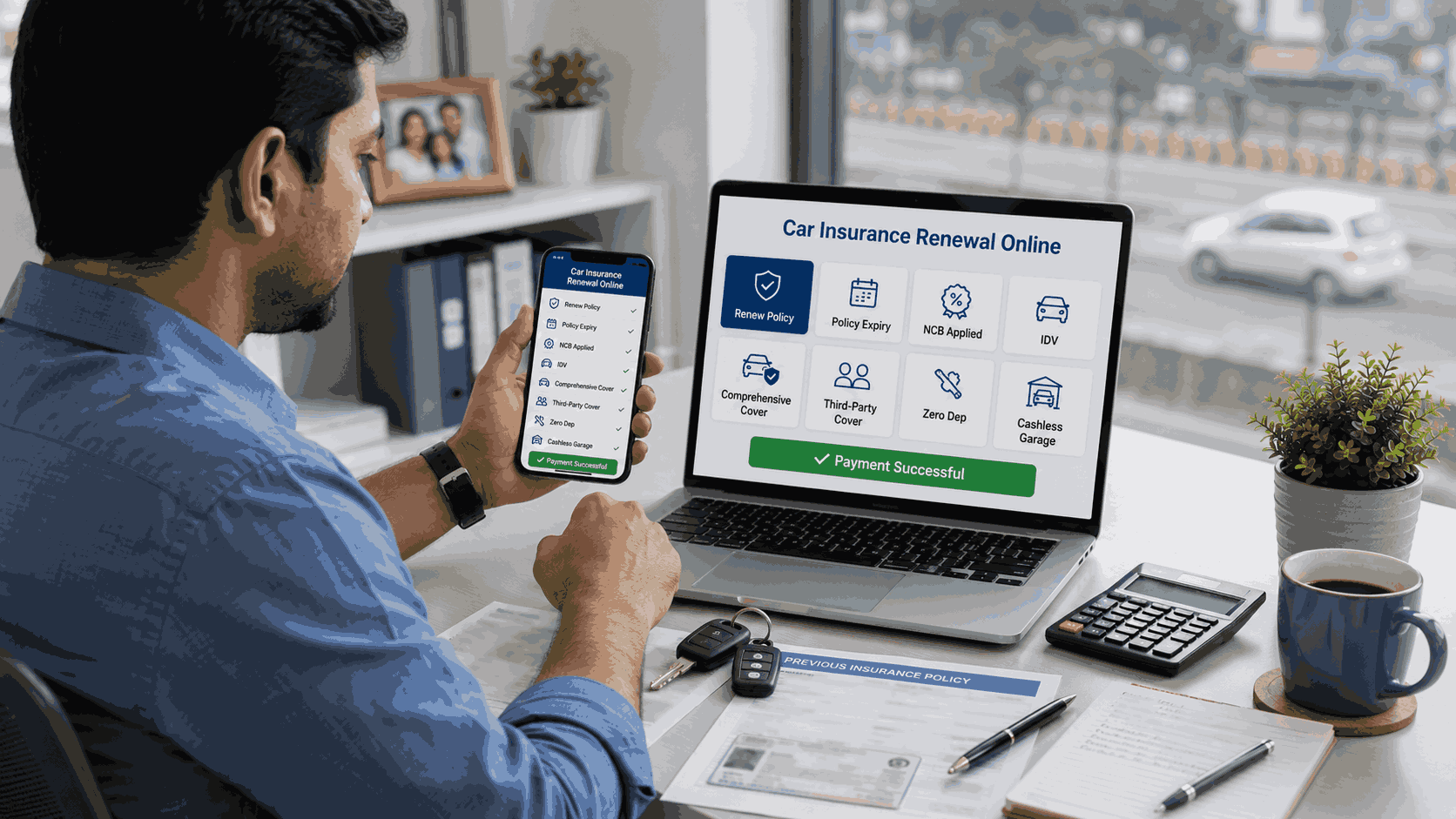
Common Insurance Challenges for Behavioral Health Providers and How to Prevent Them

FREE SEO Topical Map Generator: Find Your Next Content Ideas
Behavioral health providers help patients manage mental health, emotional concerns, substance use issues, and long-term care needs. While patient care is the main priority, insurance billing can become one of the biggest challenges for behavioral health practices.
Behavioral health billing often includes payer-specific rules, prior authorizations, session-based coding, medical necessity requirements, credentialing, and detailed documentation. If these areas are not handled correctly, providers may face claim denials, delayed payments, underpayments, and revenue loss.
Behavioral health practices across the U.S., including those searching for Medical Billing Service in Minnesota, need a strong billing process to prevent insurance delays and protect practice revenue.
Providers Care Billing LLC helps behavioral health and medical practices manage billing, coding, denial management, AR follow-up, credentialing, and complete RCM services. With transparent pricing starting at 2.49%, a 98.71% clean claims submission rate, and 98.25% first-pass acceptance, the company helps providers reduce billing stress and focus more on patient care.
Why Insurance Billing Is Challenging for Behavioral Health Providers
Insurance billing for behavioral health is often more complex than many providers expect. Each payer may have different rules for coverage, authorization, documentation, session length, and reimbursement.
For providers comparing Medical Billing Services in Minnesota, payer-specific rules, authorizations, and documentation requirements can make behavioral health billing more complex.
A small mistake in patient information, coding, eligibility verification, or documentation can delay payment or cause a claim denial.
Common behavioral health billing challenges include:
- Missing prior authorizations
- Incorrect CPT codes
- Incomplete documentation
- Eligibility verification issues
- Medical necessity questions
- Credentialing problems
- Underpaid claims
- Slow payer responses
Without a strong billing workflow, these issues can affect cash flow and create extra administrative pressure.
Challenge 1: Eligibility Verification Errors
Eligibility verification is one of the first steps in preventing insurance problems. A patient may have insurance, but the plan may not cover specific behavioral health services. In some cases, coverage may be inactive, limited, or tied to strict payer rules.
Eligibility errors can happen because of:
- Wrong member ID
- Inactive coverage
- Out-of-network benefits
- High deductibles
- Copay changes
- Coverage limits
- Plan restrictions
To prevent this issue, practices should verify benefits before every visit. Staff should confirm active coverage, copays, deductibles, authorization needs, and behavioral health benefits before services are provided.
Challenge 2: Prior Authorization Problems
Many insurance plans require prior authorization for behavioral health services. This is common for ongoing therapy, psychological testing, intensive outpatient programs, and certain treatment plans.
If authorization is missing, expired, or not linked correctly to the claim, the payer may deny payment.
To prevent authorization-related denials, practices should:
Check authorization requirements before treatment
- Track approval dates
- Monitor approved session limits
- Renew authorizations on time
- Keep authorization numbers in billing records
- Confirm payer-specific rules
A clear authorization tracking system helps reduce avoidable claim denials.
Challenge 3: Incorrect Coding
Coding mistakes are another common reason behavioral health claims are denied. Behavioral health coding may depend on session length, service type, provider type, place of service, and payer guidelines.
Common coding problems include:
- Wrong CPT code selection
- Missing modifiers
- Incorrect diagnosis codes
- Codes that do not match documentation
- Outdated codes
- Wrong place-of-service codes
To prevent coding errors, billing teams should review documentation carefully and stay updated with payer rules. Accurate coding supports cleaner claims and faster reimbursement.
Challenge 4: Weak Documentation
Documentation is very important in behavioral health billing. Insurance companies often require clear proof that services were medically necessary and properly provided.
Weak documentation can lead to denials, audits, payment delays, or requests for more information.
Strong documentation should include:
- Patient diagnosis
- Treatment planSession notes
- Medical necessity details
- Progress updates
- Service date and duration
- Provider signature
- Relevant clinical information
Complete documentation helps support the claim and protects the provider during payer review.
Challenge 5: Medical Necessity Denials
Medical necessity denials happen when a payer believes the service was not clearly needed based on the documentation provided. This does not always mean the care was unnecessary. Often, it means the notes did not explain the need clearly enough.
Behavioral health providers can reduce this risk by connecting the diagnosis, symptoms, treatment goals, session notes, and progress updates in a clear way.
The documentation should explain why the patient needs treatment, what progress is being made, and why continued care is appropriate.
Challenge 6: Credentialing and Enrollment Issues
Credentialing issues can stop a provider from getting paid. If a provider is not properly enrolled with a payer, claims may be denied even when the service was performed correctly.
Common credentialing problems include:
- Incomplete payer applications
- Expired licenses
- Outdated CAQH profiles
- Wrong NPI details
- Incorrect tax ID information
- Delayed payer approval
- Missed re-credentialing deadlines
To avoid these issues, practices should keep provider records updated and monitor payer enrollment status. Outsourcing credentialing can also help reduce errors and delays.
Challenge 7: Claim Denials and Slow Follow-Up
Claim denials are common in behavioral health billing, but they should never be ignored. If denied claims are not corrected and followed up quickly, practices can lose revenue.
Denials may happen because of eligibility errors, missing authorizations, incorrect codes, weak documentation, or payer processing issues.
A strong denial management process should include tracking denial reasons, correcting claims quickly, appealing when needed, and reviewing denial patterns to prevent repeat issues.
Challenge 8: Underpayments from Insurance Companies
Sometimes claims are paid, but the payment amount is lower than expected. These underpayments can reduce practice revenue over time if they are not reviewed.
Underpayments may happen because of:
- Contract rate issues
- Incorrect payer processing
- Missing modifiers
- Wrong fee schedule use
- Partial payments
- Coordination of benefits errors
Practices should regularly compare payments with payer contracts. This helps identify underpayments and recover missed revenue.
How Behavioral Health Providers Can Prevent Insurance Problems
Most insurance problems can be reduced with a clear billing process. The goal is to prevent errors before claims are submitted.
Behavioral health practices can improve billing performance by:
- Verifying eligibility before each visit
- Tracking prior authorizations
- Using accurate CPT and diagnosis codes
- Keeping documentation complete
- Updating credentialing records
- Reviewing denied claims regularly
- Following up on unpaid claims
- Checking payments for underpayments
- Working with experienced billing experts
A proactive billing process helps practices reduce denials, improve cash flow, and save staff time.
Why Outsourcing Billing Helps Behavioral Health Practices
Outsourcing billing gives behavioral health providers access to trained billing and RCM experts. Instead of managing complex payer rules alone, practices can work with a team that understands claims, denials, coding, credentialing, and AR follow-up.
A trusted Medical Billing company in Minnesota can help behavioral health providers reduce claim errors, manage denials, and improve cash flow.
Outsourcing can help practices:
- Reduce administrative workload
- Improve claim accuracy
- Lower denial rates
- Speed up payments
- Improve cash flow
- Reduce staff stress
- Manage credentialing better
- Focus more on patient care
For many behavioral health providers, outsourcing is not only about saving time. It is also about protecting revenue and improving financial performance.
Why Choose Providers Care Billing LLC?
Providers Care Billing LLC is a leading U.S. medical billing and revenue cycle management firm serving healthcare practices nationwide. The company provides complete billing, coding, denial management, AR follow-up, credentialing, and RCM solutions.
Among many medical billing companies in minnesota, Providers Care Billing LLC stands out with transparent pricing, complete RCM support, and strong clean claim performance.
The company is known for:
- Transparent pricing starting at 2.49%
- 98.71% clean claims submission rate
- 98.25% first-pass acceptance
- Complete medical billing support
- Expert coding services
- Denial management
- AR follow-up
- Credentialing support
- End-to-end RCM services
With reliable and compliant billing solutions, Providers Care Billing LLC helps providers spend less time on insurance problems and more time supporting patients.
Final Thoughts
Insurance challenges are common in behavioral health billing, but many of them can be prevented with the right process. Eligibility errors, missing authorizations, coding mistakes, weak documentation, credentialing issues, claim denials, and underpayments can all affect revenue.
A strong billing workflow helps behavioral health practices submit cleaner claims, reduce denials, speed up payments, and improve cash flow.
Providers Care Billing LLC offers complete billing and revenue cycle support to help behavioral health practices manage insurance challenges with confidence.
Contact Us today to reduce billing stress, improve reimbursements, and protect your practice revenue.
FAQs
What are the most common insurance challenges for behavioral health providers?
The most common challenges include eligibility errors, missing prior authorizations, coding mistakes, weak documentation, medical necessity denials, credentialing issues, and delayed claim follow-up.
Why do behavioral health claims get denied?
Behavioral health claims are often denied because of incorrect codes, missing authorization, inactive insurance, incomplete documentation, or provider enrollment problems.
How can behavioral health providers reduce claim denials?
Providers can reduce denials by verifying eligibility, tracking authorizations, using correct codes, documenting medical necessity, and following up on denied claims quickly.
Why is documentation important in behavioral health billing?
Documentation supports medical necessity and proves that the service was provided correctly. Strong notes help reduce denials and protect the provider during payer reviews.
How does Providers Care Billing LLC help behavioral health practices?
Providers Care Billing LLC helps with billing, coding, denial management, AR follow-up, credentialing, and complete RCM services to improve reimbursements and reduce administrative stress.