Cosmelan Peel Reviews: Real Results, Risks, Timeline, and Aftercare
Get a free topical map and start building content authority today.
The most searched phrase around this treatment is Cosmelan peel reviews, and for good reason: prospective patients want clear information about results, downtime, and risks before booking. This article compiles real-world outcomes, professional guidance, and a practical checklist to evaluate whether Cosmelan is appropriate for specific hyperpigmentation concerns.
- Intent: Commercial Investigation
- What Cosmelan targets: melasma and stubborn post-inflammatory hyperpigmentation via professional depigmentation peel protocols.
- Typical timeline: immediate peeling for 1–2 weeks, progressive lightening over 3–6 months with maintenance required.
- Key trade-offs: strong pigment reduction potential versus significant downtime, strict aftercare, and variable results by skin type.
Cosmelan peel reviews: what users and clinicians report
Patient and clinician reports in Cosmelan peel reviews commonly note substantial lightening of melasma patches and post-inflammatory hyperpigmentation when protocols are followed closely. Results are most consistent when treatments are performed by trained professionals, combined with daily sun protection, and followed by maintenance topical therapy.
How Cosmelan works and when it’s used
Cosmelan is a professional depot depigmentation method that combines an in-office mask with a follow-up topical regimen to reduce melanogenesis. It’s intended for moderate-to-severe hyperpigmentation, especially melasma, lentigines, and resistant post-inflammatory pigment. Treatment works by inhibiting melanin synthesis, accelerating epidermal turnover, and stabilizing pigment over months.
Clinical context and safety standards
Dermatology societies recommend thorough evaluation before aggressive depigmentation procedures. For general guidance on chemical peels, recovery, and risk assessment, refer to the American Academy of Dermatology’s patient resources: AAD — chemical peel overview.
Realistic timeline and expected results
Typical timelines cited in Cosmelan peel reviews show:
- Days 1–7: intense peeling, redness, and crusting as the in-office mask and early topicals act.
- Weeks 2–8: visible lightening with continued epidermal renewal; skin may remain sensitive to sun.
- Months 3–6: plateau of improvement—best results often require ongoing maintenance creams and strict photoprotection.
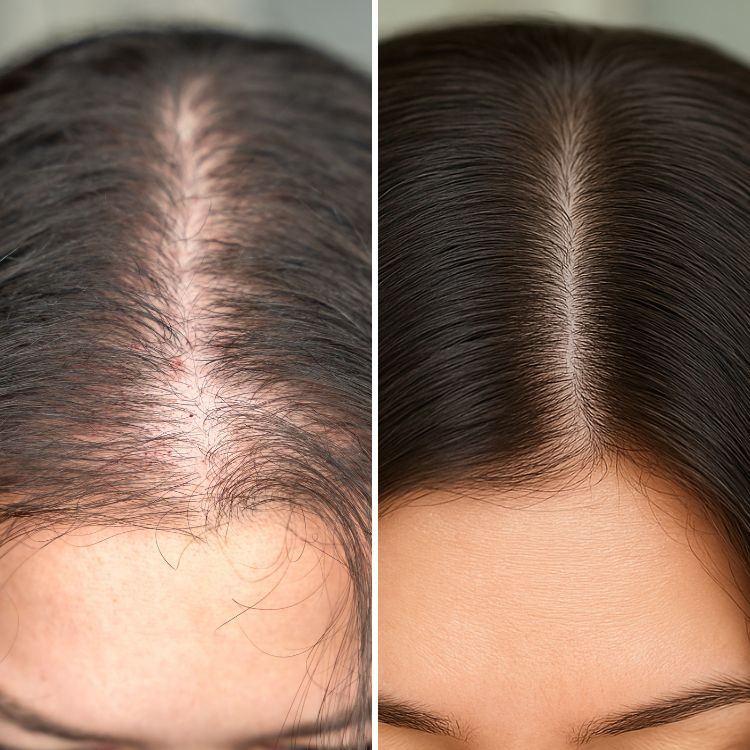
Cosmelan before and after: realistic expectations
Before and after photographs in trustworthy reviews show significant improvement in many cases, but full clearance is uncommon for deeper melasma. Expect reduction in pigment intensity and improved uniformity rather than perfect restoration to pre-pigment baseline.
Common side effects and recovery
Cosmelan peel side effects most frequently reported include transient redness, peeling, sensitivity, and temporary irritation. Less common but important risks are post-inflammatory hyperpigmentation, prolonged redness, or uneven lightening—particularly in darker skin tones if protocols are not tailored.
Risk mitigation checklist
- Pre-treatment assessment for Fitzpatrick skin type and melasma pattern.
- Patch testing for topical components when indicated.
- Clear written aftercare instructions emphasizing sunscreen and avoidance of irritants.
- Planned follow-up visits at 1–2 weeks, 1 month, and 3 months.
CLEAR Peel Review Framework (named model)
Use the CLEAR framework to evaluate any Cosmelan peel review or clinic claim:
- Consultation: documented skin exam, diagnosis, and alternatives discussed.
- Layers: explanation of what epidermal and dermal pigment is present.
- Expectations: realistic timeline and likely degree of improvement.
- Aftercare: clear regimen for topical therapy, sunscreen, and follow-up.
- Risks: explicit disclosure of possible short- and long-term side effects.
Practical aftercare and maintenance tips
Aftercare strongly influences outcomes in Cosmelan cases. Practical tips include:
- Strict broad-spectrum sunscreen (SPF 30–50) every morning and reapplication if outdoors.
- Use gentle cleansers and avoid physical exfoliants until healed.
- Follow prescribed topical maintenance agents (hydroquinone alternatives, azelaic acid, retinoids) only as directed by the treating clinician.
- Schedule follow-ups to adjust maintenance and address any rebound pigmentation promptly.
Common mistakes and trade-offs to consider
Common mistakes
- Skipping a professional consultation and self-administering strong depigmenting agents—risk of uneven results and burns.
- Poor sun protection during the recovery window, which can reverse gains and cause rebound hyperpigmentation.
- Expecting immediate, complete clearance—pigment often improves gradually over months.
Trade-offs
The main trade-off is between efficacy and intensity: Cosmelan can produce notable pigment reduction compared with gentler topical approaches, but it requires stronger downtime, stricter aftercare, and close clinical supervision. For mild pigment, gentler topical regimens may be preferable; for severe or treatment-resistant pigment, Cosmelan may be justified under specialist care.
Short real-world scenario
A 38-year-old with centrofacial melasma and Fitzpatrick III skin underwent a Cosmelan protocol. After pre-treatment counseling and sun-protection planning, the in-office mask was applied. The first week included heavy peeling and erythema, managed with prescribed soothing creams. By month three, the patient had a 50–70% reduction in pigment intensity, continued sunscreen use, and a prescribed maintenance topical combination to prevent recurrence.
Core cluster questions
- How do professional depigmentation peels work for melasma?
- What aftercare is essential to prevent pigment rebound after a chemical peel?
- Which factors predict better outcomes with depigmentation protocols?
- How does downtime compare across aggressive and conservative pigment treatments?
- What alternatives to in-office peels exist for long-term melasma management?
Practical evaluation checklist before booking
- Confirm diagnosis (melasma vs. post-inflammatory hyperpigmentation).
- Request detailed before-and-after photos from the clinic for similar skin types.
- Get written aftercare and a follow-up schedule.
- Discuss maintenance topical options and sun protection strategy.
- Make a plan for contingencies if post-procedure pigmentation worsens.
Summary and final considerations
Cosmelan peel reviews indicate that the treatment can produce meaningful pigment reduction for many patients when applied and followed correctly. The decision should weigh the potential benefit against expected downtime, strict aftercare, and the need for ongoing maintenance. A specialist evaluation and adherence to post-procedure photoprotection are critical to successful outcomes.
Are Cosmelan peel reviews accurate and trustworthy?
Cosmelan peel reviews vary in quality. Trustworthiness increases when reports include standardized photos, timeline context, clinician oversight, and clear before-and-after documentation for similar skin types. Use the CLEAR framework above to assess the reliability of any review.
How long do Cosmelan results last?
Results can last months to years with proper maintenance and strict sun protection. Recurrence of melasma is common without continued topical therapy and photoprotection.
What are typical Cosmelan peel side effects?
Common side effects include peeling, redness, and temporary irritation; less commonly, post-inflammatory hyperpigmentation or persistent erythema may occur, especially without correct aftercare.
Is Cosmelan suitable for darker skin tones?
Cosmelan can be used on darker skin but requires experienced clinicians to tailor application, reduce complication risk, and provide extended follow-up. Pre- and post-treatment regimens should be customized for Fitzpatrick IV–VI skin types.
How to verify a clinic before treatment?
Verify clinician qualifications, ask for documented similar-case results, confirm an aftercare plan, and ensure the clinic follows accepted safety protocols. If uncertain, seek a second opinion from a board-certified dermatologist.