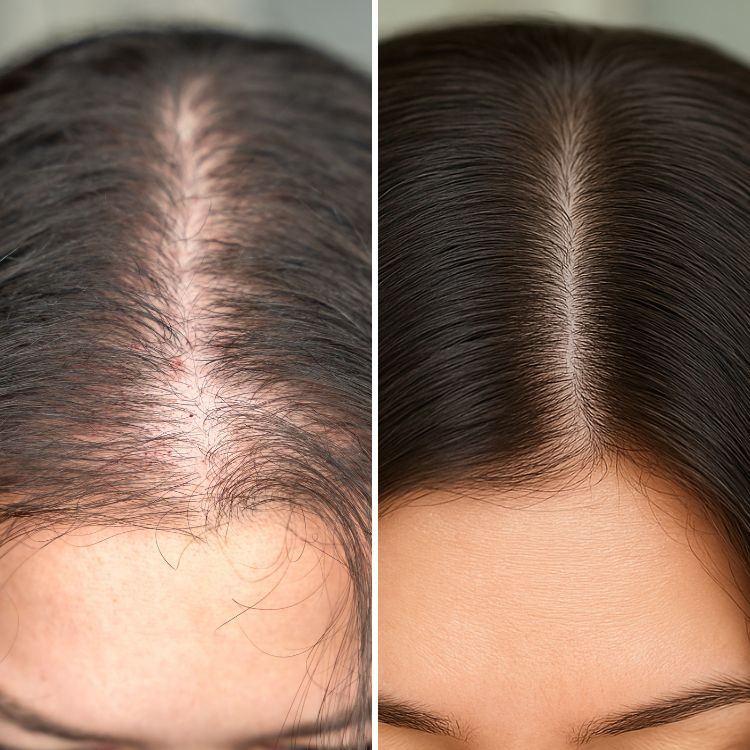
Complete Hair Transplant Guide: Procedures, Recovery, Risks, and Costs
Get a free topical map and start building content authority today.
The hair transplant is a surgical procedure to move hair follicles from a donor area to thinning or balding sites. This guide explains common methods, expected recovery, possible complications, and practical considerations for selecting a qualified surgeon or clinic.
- Common techniques include follicular unit extraction (FUE) and follicular unit transplantation (FUT).
- Recovery typically involves days to weeks of scalp tenderness, scabbing, and temporary shedding of transplanted hairs.
- Risks include infection, scarring, poor graft survival, and unnatural hairline if planning is inadequate.
- Clinic accreditation, surgeon experience, and realistic expectations influence outcomes.
Hair transplant: Overview
Hair transplant procedures are designed to restore hair density by relocating hair-bearing follicles. The most widely used methods are follicular unit extraction (FUE) and follicular unit transplantation (FUT), also called strip surgery. Techniques may be combined with adjuncts such as platelet-rich plasma (PRP) to potentially support graft survival. Regulatory bodies and professional societies, including surgical boards and hair restoration organizations, provide guidance on standards and training.
Who may be considered for a transplant
Typical candidates
People with pattern hair loss who have adequate donor hair (usually at the back and sides of the scalp) are common candidates. Candidates often are adults with stable hair loss, realistic expectations, and general medical suitability for minor surgery. Factors such as age, extent of hair loss, donor hair density, and overall health influence candidacy.
When alternative options are appropriate
Non-surgical approaches — topical treatments, prescription medications, cosmetic concealers, and hairpieces — may be recommended alone or before considering surgery. Consultation with a qualified clinician can clarify whether surgery is likely to achieve the desired outcome.
Methods and how they differ
FUE (Follicular Unit Extraction)
FUE involves harvesting individual follicular units using small punches. Advantages may include smaller, dot-like scars and quicker initial healing. The procedure can be labor-intensive and may require shaving of the donor area.
FUT (Follicular Unit Transplantation / strip)
FUT removes a narrow strip of scalp from the donor area; technicians dissect it into grafts. This method can yield a high number of grafts in a single session but results in a linear scar that may be concealed by hair if long enough.
Other approaches
Robotic assistance, sapphire blades, or manual microdissection are technological variations that aim to improve graft handling and placement. Scientific literature and clinical guidelines are evolving; outcomes depend heavily on surgical skill and graft handling.
What to expect during the procedure
Typical steps
Procedures usually occur under local anesthesia and may take several hours to a full day depending on graft number. Steps include donor harvest, graft preparation, recipient site creation, and placement of grafts. Postoperative dressings and instructions are provided before discharge.
Graft survival and hair growth timeline
Early shedding of transplanted hairs within weeks is common; new growth often begins around three to four months and improves over 6–12 months. Final cosmetic results can take up to 12–18 months in some cases.
Recovery, aftercare, and expected outcomes
Early recovery
Expect swelling, mild pain, scabbing, and numbness in treated areas. Specific aftercare instructions typically cover wound cleaning, avoiding strenuous activity, and how to sleep to protect grafts.
Long-term care and follow-up
Follow-up appointments assess healing and hair growth. Ongoing treatments to stabilize native hair (for example, topical or systemic therapies) may be discussed by a clinician to prolong overall results.
Risks, complications, and realistic expectations
Common complications include infection, bleeding, poor graft take, scarring, numbness, and an appearance that may not meet expectations. Patient selection, surgical technique, and postoperative care influence complication rates. Professional organizations recommend clear informed consent and documentation of likely outcomes.
Choosing a clinic and surgeon
Credentials and experience
Seek a surgeon with specific training and documented experience in hair restoration. Clinic accreditation, before-and-after portfolios, patient reviews, and transparent discussion of risks and costs are relevant factors.
Questions to ask
Relevant questions include details about the proposed technique, expected graft numbers, anesthesia plans, complication rates, follow-up schedule, and whether an assistant or team performs critical steps. Cost transparency and written treatment plans are important.
Costs and insurance considerations
Hair transplant costs vary by technique, number of grafts, geographic location, and clinic. Cosmetic hair restoration is commonly not covered by health insurance, though coverage policies vary by jurisdiction and insurer.
Evidence and regulation
Clinical research on techniques, graft survival, and adjunctive therapies is available in medical literature. Professional societies, surgical boards, and national health services provide guidance on practice standards. For general public information on hair transplant effectiveness and considerations, see the NHS overview on hair transplant surgery here.
Final considerations
Outcomes depend on realistic expectations, surgeon skill, adequate donor supply, and appropriate postoperative care. Consultation with a qualified clinician and review of independent resources are recommended before making decisions about surgery.
FAQ
What is a hair transplant and how does it work?
A hair transplant relocates hair follicles from a donor area to areas of thinning or baldness. Techniques like FUE and FUT differ in how grafts are harvested and placed; transplanted follicles continue to grow hair in most cases after an initial shedding phase.
How long is recovery after a transplant?
Initial recovery is often a few days to two weeks for most discomfort and scabbing. Visible improvement in density usually appears over several months, with final results commonly assessed at 9–12 months.
What are the main risks of hair transplant surgery?
Risks include infection, bleeding, scarring, poor graft survival, numbness, and unsatisfactory cosmetic results. Proper patient selection and technique can reduce but not eliminate risks.
How should a clinic and surgeon be chosen?
Consider surgeon credentials, experience in hair restoration, clinic accreditation, clear disclosure of costs and risks, documented results, and detailed preoperative planning. Seek multiple opinions if uncertain.