Remote Patient Monitoring: Practical Guide to Benefits, Setup, and Best Practices
Get a free topical map and start building content authority today.
Remote patient monitoring is changing how chronic disease, post-discharge care, and preventive medicine are delivered by collecting health data outside traditional clinical settings and using it to guide timely care. This guide explains what remote patient monitoring looks like in practice, how to set up a reliable program, and the trade-offs clinicians and health systems face when scaling RPM solutions.
- Remote patient monitoring (RPM) uses devices and software to capture patient data outside the clinic and feed it into care workflows.
- Key benefits: improved chronic care, fewer readmissions, earlier intervention, and better patient engagement.
- Critical success factors: device selection, clinical protocols, EHR integration, data governance, and reimbursement strategy.
Detected intent: Informational
Remote patient monitoring: what it is and why it matters
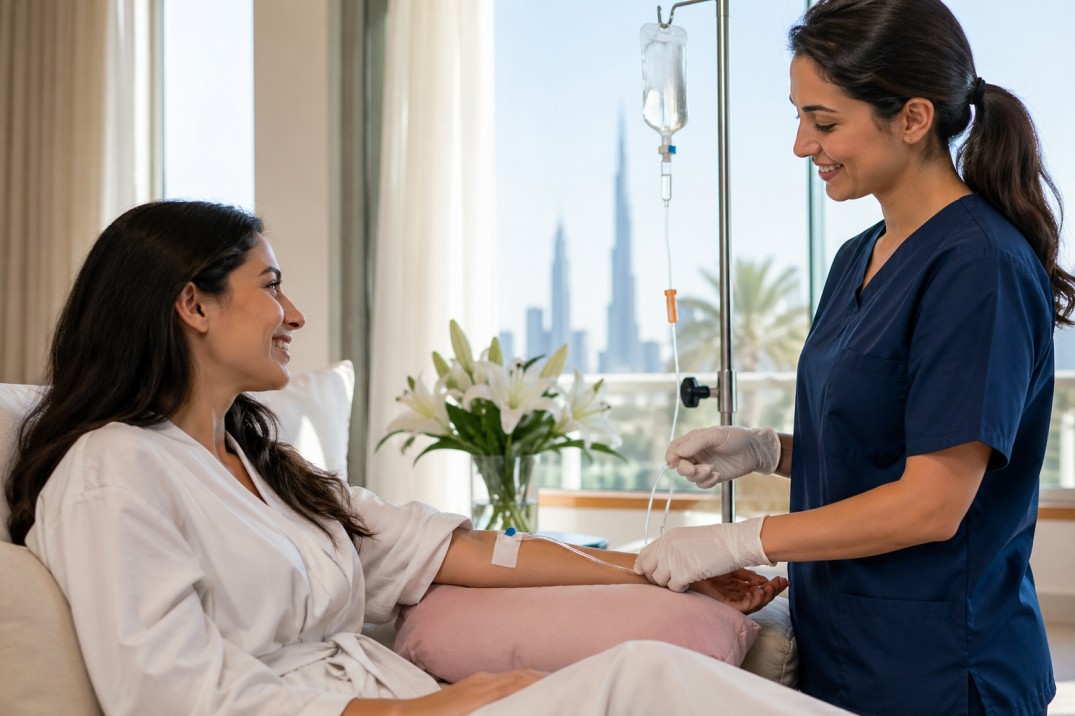
Remote patient monitoring (RPM) refers to the continuous or scheduled collection of biometric, symptom, or activity data from patients at home or in the community, transmitted to clinicians for review and action. RPM can include pulse oximetry, blood pressure, glucose, weight scales, wearable activity trackers, and patient-reported outcomes. When combined with clinical workflows, RPM helps detect deterioration earlier, reduce avoidable visits, and support value-based care programs.
How RPM works — core components
Devices and connectivity
RPM devices and sensors capture physiologic signals (for example, blood pressure cuffs, glucometers, pulse oximeters, and wearable activity trackers). Devices may connect via Bluetooth to a smartphone app or transmit directly over cellular networks. Prioritize devices with clinical accuracy, clear data standards, and vendor support for firmware updates.
Data aggregation and integration
Data flows from devices into a platform that normalizes measurements, applies algorithms or thresholds, and delivers alerts to clinicians. Integration with electronic health records (EHRs) using standards such as HL7 FHIR avoids siloed dashboards and makes RPM data part of the medical record. Define clear data retention and privacy policies consistent with HIPAA and regional regulations.
Clinical workflows and roles
Successful RPM requires defined protocols: who reviews alerts, triage thresholds, and escalation steps. Typical models use nurses or care managers to monitor incoming data and route exceptions to physicians. Embedding RPM into care pathways—for example, heart failure clinics or post-surgical follow-up—produces the most measurable benefits.
RPM Readiness Checklist (5-Point RPM Readiness Checklist)
- Population fit: Identify patient groups with clear monitoring needs (e.g., heart failure, COPD, uncontrolled diabetes).
- Device strategy: Standardize on clinically validated devices and single-vendor or interoperable options to simplify support.
- Data and EHR integration: Ensure data maps into the EHR using FHIR/HL7 and that alerts fit existing workflows.
- Clinical protocols: Define thresholds, response times, and responsible staff for escalations.
- Reimbursement and finance: Verify billing codes, coverage, and ROI expectations (for example, checking remote physiologic monitoring reimbursement rules and payer policies).
Practical implementation steps
Step-by-step actions to launch RPM
- Define the clinical use-case and measurable goals (reduce readmissions by X%, improve A1c, etc.).
- Choose validated devices and confirm connectivity options for the patient population (smartphone vs. cellular).
- Implement a data platform that supports FHIR and can push summarized data to the EHR.
- Pilot with a small cohort, collect user feedback, and measure clinical and operational outcomes.
- Scale with standardized onboarding, training materials, and clear reimbursement tracking.
Real-world example
A community hospital piloted RPM for heart failure patients discharged after exacerbation. Patients received a Bluetooth weight scale and blood pressure cuff that transmitted daily readings. A nurse reviewed automated alerts for rapid weight gain and coached medication adherence via phone. Within six months the program reduced 30-day readmissions by 18% and improved patient satisfaction scores. Critical factors were reliable cellular connectivity for patients without smartphones and an escalation protocol that routed urgent alerts to clinicians within two hours.
Practical tips for clinicians and program managers
- Start with a narrow use-case and clear outcome metrics to measure ROI and clinical impact.
- Standardize devices where possible—device diversity increases support burden and data variability.
- Train patients with short, visual guides and a single helpline for technical support to reduce drop-off.
- Automate low-risk alerts and reserve clinician time for actionable exceptions to avoid alarm fatigue.
- Partner with compliance and security teams early to align with HIPAA and local regulations.
Trade-offs and common mistakes
Trade-offs to consider
Choosing broad device compatibility increases patient reach but complicates integration and support. Prioritizing the most accurate medical devices raises costs but yields more reliable clinical decisions. Fully automated alerting speeds response but risks false positives—balanced thresholds and periodic algorithm tuning are necessary.
Common mistakes
- Implementing RPM without defined clinical workflows—data without action produces noise, not value.
- Failing to address digital divide issues—devices that rely on smartphones can exclude older or low-income patients.
- Neglecting interoperability—siloed dashboards limit clinician adoption and long-term sustainability.
Regulatory, standards, and reimbursement notes
Regulatory guidance and reimbursement rules vary by country and payer. Refer to recognized regulatory resources for guidance on device classification and digital health best practices. For example, the FDA maintains a Digital Health Center of Excellence that provides resources on digital health technologies and regulatory considerations: FDA Digital Health.
Core cluster questions
- How is remote patient monitoring reimbursed by payers?
- What devices are clinically validated for RPM in heart failure?
- How to integrate RPM data into an EHR using FHIR?
- Which patient populations benefit most from continuous vs. scheduled monitoring?
- How to design clinical escalation protocols for RPM alerts?
Metrics to track
Track clinical outcomes (readmissions, A1c, COPD exacerbations), engagement metrics (adherence to daily readings), operational metrics (alert volume per patient), and financial metrics (billing capture, cost per patient). Regularly review these KPIs to iterate on thresholds, patient selection, and staffing models.
Legal and privacy checklist
Confirm business associate agreements for vendors, encrypt data in transit and at rest, maintain transparent patient consent forms, and align retention policies with clinical and legal requirements.
Next steps for teams
Begin with a 90-day pilot, use the 5-Point RPM Readiness Checklist above, and measure both clinical and operational outcomes. Use integration standards (HL7/FHIR) to future-proof the program and plan for gradual scale-up based on early wins.
What is remote patient monitoring?
Remote patient monitoring is the collection and transmission of patient health data from outside clinical settings to clinicians who use the data to inform care decisions. It supports chronic disease management, post-discharge follow-up, and preventive interventions.
How does remote physiologic monitoring reimbursement work?
Reimbursement for RPM varies by payer and jurisdiction. Many programs require documented patient consent, defined monitoring periods, and qualified clinical staff time. Verify local billing codes and payer policies before scaling.
Which patients benefit most from RPM?
Patients with conditions that show measurable physiologic signs—heart failure, COPD, hypertension, diabetes—often benefit most. Consider social determinants and digital access when selecting candidates.
How are RPM data integrated into clinical workflows?
Best practice is to normalize device data in a platform that maps to EHR fields via FHIR/HL7 and route alerts into existing communication channels (inbox, task lists) used by clinicians.
How to measure success for an RPM program?
Define success metrics before launch: clinical outcomes (readmissions, A1c), patient engagement (adherence), operational efficiency (alerts handled per clinician hour), and financial performance (cost per avoided admission).