Complete Dental Implants Guide: Costs, Procedure, Recovery, and Checklist
FREE SEO Topical Map Generator: Find Your Next Content Ideas
This dental implants guide explains what dental implants are, who is a candidate, the typical procedure steps, recovery timeline, cost factors, risks, and practical planning advice for anyone considering implants.
- Dental implants replace tooth roots with a titanium post, an abutment, and a crown or denture.
- Typical timeline: 3–9+ months (implant placement, osseointegration, final restoration).
- Common costs vary widely by region and treatment complexity; bone grafts and sinus lifts add time and cost.
- Use a checklist and confirm medical history, imaging, and a written treatment plan before surgery.
Detected intent: Informational
Dental implants guide: what implants are and who they help
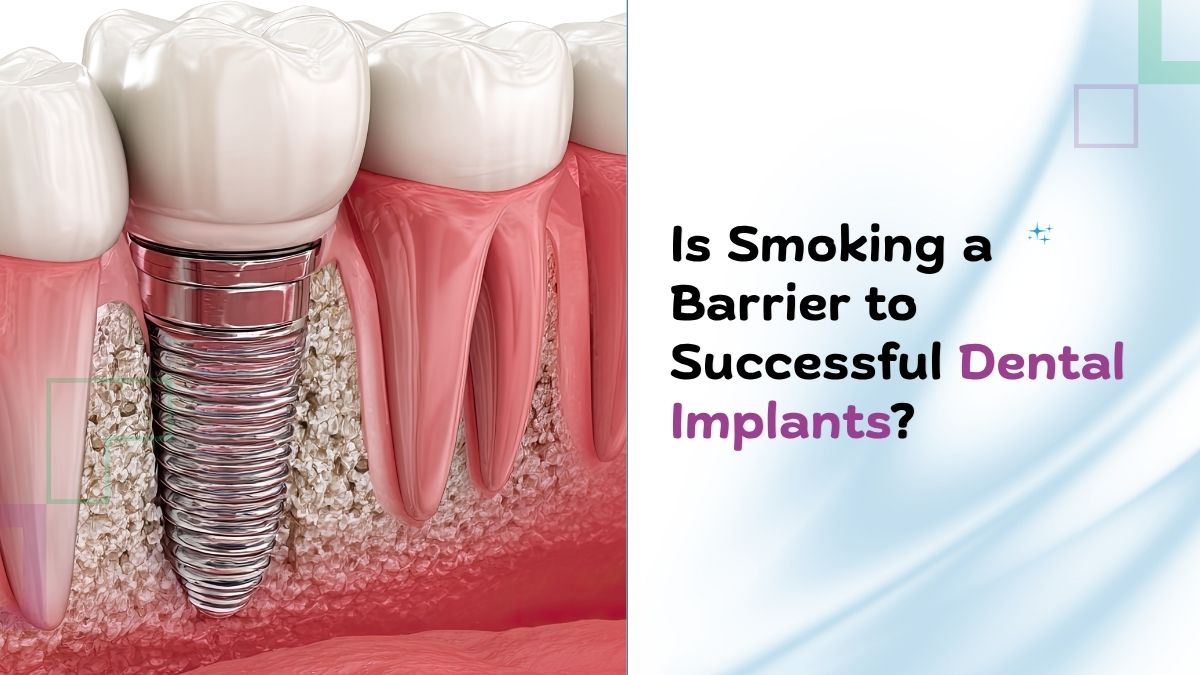
Dental implants are prosthetic tooth roots—usually titanium or titanium alloy posts—placed into the jawbone to support a dental crown, bridge, or denture. Key related terms include osseointegration (bone fusing to the implant), abutment (connects implant to the crown), and bone grafting (adds bone when natural volume is insufficient). Candidates typically include people with one or more missing teeth, good overall health, and sufficient jawbone; smoking, uncontrolled diabetes, or heavy radiation therapy to the jaw can affect candidacy.
Procedure overview and timeline
Dental implant procedure steps
Most implant treatments follow this sequence: initial consultation and 3D imaging (CBCT), medical clearance, tooth extraction if needed, implant placement surgery, healing and osseointegration (3–6 months typical), abutment placement, and final crown or prosthesis. Some cases use immediate loading (a temporary tooth same day) but that requires strict selection criteria. The phrase "dental implant procedure steps" commonly appears in patient questions because staging and timing matter for planning and cost.
Recovery timeline and aftercare
Initial post-op healing is usually 1–2 weeks for soft tissue. Full osseointegration usually takes 3–6 months for lower jaws and sometimes longer for upper jaws or grafted bone. Follow-up visits confirm stability; oral hygiene, antimicrobial rinses, and avoiding heavy chewing on a new implant in early stages support success. Discuss antibiotic and pain-control protocols with the dental provider; these vary by clinical guidelines and patient risk.
Risks, benefits, and trade-offs
Benefits
Implants preserve adjacent teeth (unlike fixed bridges that require neighboring teeth to be filed), maintain jawbone volume, and provide stable chewing and better long-term satisfaction for many patients.
Common mistakes and trade-offs
Common mistakes include skipping 3D imaging, accepting vague timelines, and underestimating the need for grafting. Trade-offs involve cost versus longevity: higher upfront cost for implants compared with removable dentures often yields better function and durability, but implants require surgery and longer treatment time. Smoking and poor oral hygiene significantly increase the risk of peri-implantitis (infection around the implant).
Costs, insurance, and practical planning
Cost factors
Cost drivers include number of implants, need for bone grafts or sinus lifts, type of final restoration (single crown vs. implant-supported denture), geographic location, and provider expertise. Insurance coverage varies; some dental plans cover part of the crown or associated procedures. For reliable clinical recommendations and public guidance, consult professional resources such as the American Dental Association.
Financing and written treatment plan
Request a written estimate and a sequenced treatment plan that lists all components, alternatives, and timelines. Confirm who does which step (periodontist/oral surgeon for placement, restorative dentist for crowns) and get medical clearance if there are systemic conditions.
IMPLANT Checklist (named framework)
Use the IMPLANT Checklist before starting treatment:
- I — Initial consult & imaging (CBCT/OPG)
- M — Medical history and medication review
- P — Preparation: extraction plan & bone grafting needs
- L — Local anesthesia and sedation plan
- A — Abutment and prosthesis selection (fixed vs removable)
- T — Timeline, costs, and follow-up schedule
Practical tips and a short real-world example
Practical tips
- Get CBCT imaging early to evaluate bone volume and sinus proximity—this reduces surprises.
- Confirm whether a staged approach (graft then implant) or immediate placement suits the clinical situation.
- Ask for a single-page written plan showing steps, responsible clinicians, and expected dates.
- Stop smoking at least several weeks before surgery and continue abstinence during healing to improve success rates.
Short scenario
Example: A 58-year-old patient with a failed molar undergoes extraction, horizontal ridge preservation bone graft, and implant placement 4 months later. Osseointegration completes after 3 months; an abutment and crown are placed at month 7. The IMPLANT Checklist was used to confirm imaging, medical clearance for controlled hypertension, and the final cost estimate included the graft and crown.
Core cluster questions
- How long does the dental implant healing process take?
- What are the signs of implant failure or infection?
- When is a bone graft required before implant placement?
- What differences exist between single dental implants and implant-supported dentures?
- How should oral hygiene be adjusted after implant surgery?
Common mistakes to avoid
Avoid providers who cannot supply a clear, itemized treatment plan, skip necessary imaging, or promise unrealistic timelines. Do not ignore systemic health factors—uncontrolled diabetes or certain medications (bisphosphonates) can change risk profiles. Finally, be cautious about discount offers that omit key steps like grafting or a proper prosthetic workflow.
FAQ
What does this dental implants guide include?
This guide covers definitions, procedure steps, recovery timeline, cost factors, the IMPLANT checklist, practical tips, a short case scenario, core cluster questions for follow-up reading, and common mistakes to avoid.
How long do dental implants last?
With good oral hygiene, professional maintenance, and absence of complicating health issues, implants can last decades; restorations (crowns) may need replacement every 10–15 years depending on wear.
Are dental implants painful?
Most patients report manageable pain controlled with over-the-counter or prescribed analgesics. Local anesthesia is used during surgery and most discomfort subsides within a few days to two weeks for soft tissue healing; longer discomfort suggests complications and should be evaluated.
When is a bone graft or sinus lift necessary?
Bone grafting or sinus lift is necessary when jawbone volume is insufficient to securely anchor an implant. 3D imaging determines bone quantity and the need for augmentation; grafting extends timelines but improves long-term outcomes.
Can smoking affect implant success?
Yes. Smoking is strongly associated with higher rates of implant failure and peri-implant infection. Quitting before and after surgery materially improves the prognosis.