Videonystagmography (VNG): Purpose, Procedure, and What to Expect
👉 Best IPTV Services 2026 – 10,000+ Channels, 4K Quality – Start Free Trial Now
Videonystagmography (VNG) test is a diagnostic exam that records eye movements to evaluate balance and vestibular function. The test is commonly used when a person reports vertigo, dizziness, unsteadiness, or recurrent falls. Results help clinicians identify whether symptoms originate from the inner ear, central nervous system, or other causes.
- Purpose: Assess eye movements to identify vestibular (inner ear) and neurological causes of dizziness.
- Duration: Typically 30–90 minutes depending on which components are performed.
- Components: Goggle-based infrared video recording, positional testing, and caloric testing.
- Preparation: Avoid sedatives and some vestibular-suppressant medications as instructed by the clinician.
- Follow-up: Results interpreted by an audiologist, neurotologist, or ENT specialist; further tests may be recommended.
What is a videonystagmography (VNG) test?
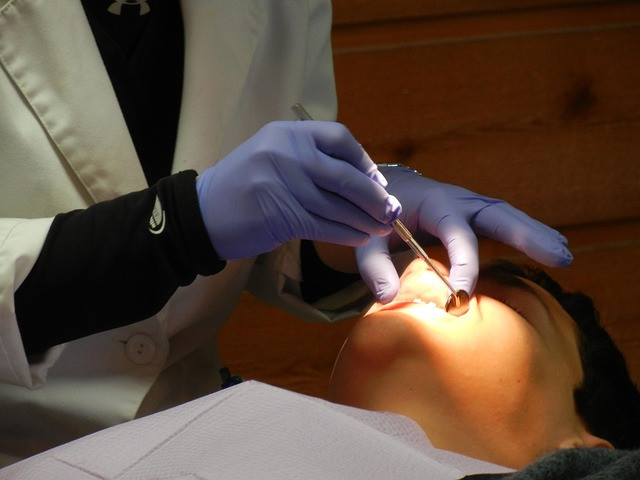
A videonystagmography (VNG) test records involuntary eye movements (nystagmus) using infrared cameras mounted in lightweight goggles. Eye movement patterns are analyzed while the patient follows visual targets, changes head or body position, or receives warm and cold air or water stimulation in the ears (caloric testing). Nystagmus patterns can indicate peripheral vestibular dysfunction (inner ear) or central causes (brainstem or cerebellum).
Why clinicians order a VNG
Common reasons to order a VNG include:
- Recurrent or persistent vertigo or spinning sensations
- Unexplained imbalance or falls
- Sudden onset of dizziness with no clear cause
- Follow-up after head injury to assess vestibular impact
- Pre-surgical or post-surgical evaluation of vestibular function
Before the test: preparation and precautions
Medication and activity
Certain medications can suppress vestibular responses and affect results. Examples include antihistamines, benzodiazepines, some anti-nausea drugs, and vestibular suppressants. A clinician will provide instructions about which medications to withhold and for how long. Avoid alcohol for at least 24 hours before testing. Eating a light meal and wearing comfortable clothing is recommended.
Medical history and consent
Provide a complete history of symptoms, recent illnesses, past ear or neurologic conditions, and a list of current medications. A clinician will explain possible sensations during testing and obtain consent. Inform the testing team of pregnancy, recent ear surgery, severe neck or back problems, or known reactions to cold stimulation.
What happens during a VNG test?
The VNG typically includes three main components: oculomotor testing, positional testing, and caloric testing. The exact sequence varies by clinic and patient needs.
Oculomotor testing
While wearing the goggles, the patient follows visual targets (e.g., moving lights) to assess smooth pursuit, saccades (quick eye movements), and tracking. This helps identify abnormalities in eye movement control that may suggest central nervous system involvement.
Positional and positioning testing
Various head and body positions are used to provoke or observe nystagmus. Examples include lying back, turning the head to each side, or the Dix-Hallpike maneuver when benign paroxysmal positional vertigo (BPPV) is suspected. The goggles record any resulting nystagmus and its direction, speed, and duration.
Caloric testing
Caloric testing separately stimulates each ear by introducing warm and cold air or water into the ear canal while the head is reclined. The temperature difference induces a predictable eye movement response in a healthy vestibular system. Comparing responses between ears helps detect unilateral weakness or asymmetry. Caloric testing can cause brief vertigo, nausea, or sweating; staff remain present to monitor comfort and safety.
Interpreting results and next steps
VNG recordings are analyzed for presence, direction, frequency, and velocity of nystagmus. Patterns consistent with peripheral vestibular dysfunction differ from those suggesting central causes. Reported findings are combined with clinical examination, imaging (if ordered), and other tests such as vestibular-evoked myogenic potentials (VEMP) or audiometry.
Who interprets the results?
Results are typically reviewed by an audiologist, neurologist, or otolaryngologist (ENT) with vestibular expertise. Clinical correlation is essential; a normal VNG does not rule out all causes of dizziness, and abnormal findings require clinical interpretation in context.
Risks, limitations, and alternatives
VNG is generally safe but can provoke temporary vertigo, nausea, or vomiting during testing. Individuals with certain ear or vascular conditions may need modified protocols. Limitations include reduced sensitivity for some vestibular disorders and difficulty performing parts of the test if neck or spine mobility is limited. Alternative or complementary tests include rotational chair testing, VEMP, posturography, and MRI when central pathology is suspected.
Clinical guidance and resources
Guidance on vestibular disorders and balance testing is provided by professional organizations and government health agencies. For general information about vestibular conditions and diagnostic approaches, see the National Institute on Deafness and Other Communication Disorders (NIDCD): https://www.nidcd.nih.gov/health/vestibular-disorders. Professional societies such as the American Academy of Otolaryngology—Head and Neck Surgery and audiology associations publish clinical resources and practice parameters.
Practical tips for patients
- Ask the clinic which medications to stop and how long before the test.
- Bring a list of current medications and any recent diagnostic reports.
- Arrange transportation if vestibular symptoms are severe afterward.
- Plan time for possible recovery from transient symptoms after caloric stimulation.
What does a videonystagmography (VNG) test measure?
The VNG measures involuntary eye movements (nystagmus) in response to visual tracking, positional changes, and thermal stimulation of the inner ear. Metrics include nystagmus direction, frequency, and slow-phase velocity, which help localize vestibular dysfunction.
How long does the VNG take and will it make dizziness worse?
Testing commonly lasts 30–90 minutes. Some parts, especially caloric testing, may temporarily increase dizziness or nausea; these effects typically resolve within minutes to hours. Clinical staff monitor symptoms and can pause testing if needed.
Can medication or alcohol affect the VNG?
Yes. Many vestibular-suppressant medications and recent alcohol intake can reduce responses and affect accuracy. Follow the clinic's instructions about medication withholding and abstaining from alcohol before the test.
Is VNG safe for everyone?
VNG is safe for most people, but specific medical conditions (e.g., active ear infections, recent ear surgery, or certain cardiovascular issues) may require alternative approaches or precautions. Discuss any concerns with the care team before testing.
How are VNG results used?
Results guide diagnosis and management decisions, including vestibular rehabilitation, medication options, further imaging, or referral to neurology or ENT specialists. A multidisciplinary approach often produces the most accurate assessment of dizziness and balance disorders.