Can a Hair Transplant Permanently Cure Baldness? Realistic Outcomes and Options
Get a free topical map and start building content authority today.
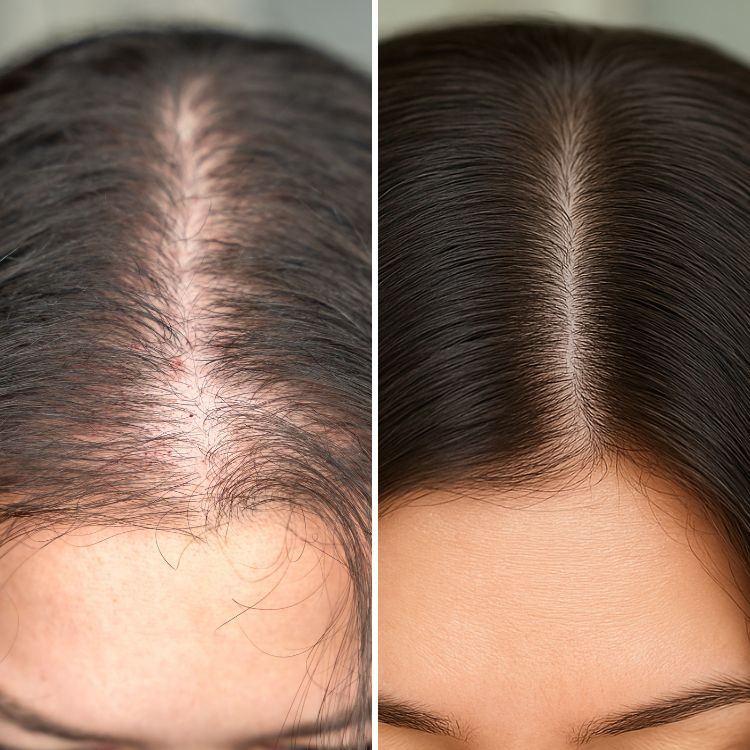
Most questions about hair restoration start with a simple search phrase: does hair transplant cure baldness permanently? The short answer is nuanced. Hair transplants move hair from donor areas to thinning or bald areas, and in many cases transplanted hairs are long-lasting. However, long-term success depends on factors such as underlying hair-loss type, donor supply, ongoing medical care, and realistic expectations.
- Detected intent: Informational
- Hair transplants can provide permanent graft survival, but they do not stop genetic hair loss elsewhere.
- Best outcomes require proper candidacy assessment, medical management, and realistic expectations.
- Consider alternatives and maintenance plans if diffuse or progressive hair loss is present.
Does hair transplant cure baldness permanently?
The phrase "does hair transplant cure baldness permanently" is a high-intent question that asks whether a single procedure eliminates future hair loss. Transplanted hair follicles typically retain their original genetic resistance to hair loss when moved from the back or sides of the scalp (donor area) to the top. That means transplanted grafts can survive for many years — often decades — which is why surgery is described as a form of permanent hair restoration. However, this permanence applies to the transplanted follicles, not to native follicles susceptible to androgenetic alopecia (pattern hair loss).
How hair transplants work and what "permanent" means
Common techniques include follicular unit extraction (FUE) and follicular unit transplantation (FUT). Both harvest donor follicles that are typically resistant to dihydrotestosterone (DHT) and implant them into thinning sites. "Permanent" in clinical terms usually refers to graft survival: if the graft takes, those implanted follicles continue to produce hair. But progressive hair loss can thin surrounding native hair, changing the overall cosmetic appearance over time.
Related terms and entities
- Permanent hair restoration (secondary keyword)
- Androgenetic alopecia, DHT, donor dominance
- FUE vs FUT differences (secondary keyword)
- Hair transplant candidacy and maintenance
Who is a good candidate? The PRIME candidacy framework
Use the PRIME framework to evaluate candidacy before considering surgery:
- P — Pattern: Stable, predictable pattern hair loss (Norwood Class II–V) favors predictable planning.
- R — Reservoir (donor supply): Adequate donor density at the occipital and parietal scalp.
- I — Illness & medications: No uncontrolled systemic disease or medications that prevent healing.
- M — Motivation & expectations: Realistic goals about density, scarring, and possible future procedures.
- E — Existing treatments: Prior or ongoing medical treatments (minoxidil, finasteride) and willingness to continue them.
Short real-world scenario
Example: A 35-year-old male with Norwood III pattern has good donor density and has used finasteride for two years with stabilization. Surgery is planned to rebuild the frontal hairline with FUE. Transplanted grafts survive long-term, but the patient is advised to continue finasteride to reduce future loss of native hair in the crown, and to expect a possible touch-up after several years.
What to expect: timeline, results, and maintenance
Typical timeline: initial healing in 7–14 days, visible growth at 3–6 months, mature results at 9–18 months. Transplanted hair often behaves like normal hair (growth cycles, thickness) but may require medical maintenance to preserve surrounding native hair. Combining surgery with medical therapy or low-level laser therapy improves long-term appearance and reduces the need for additional transplants.
Common mistakes and trade-offs
- Expecting instant density: A single session may not achieve the pre-loss density, especially in large bald areas.
- Ignoring progressive loss: Not treating ongoing pattern baldness can leave transplanted islands of hair isolated on a thinning scalp.
- Overharvesting donor area: Aggressive harvesting can reduce future options and cause visible scarring.
- Underestimating maintenance: Avoiding medical therapy post-op can reduce the overall long-term aesthetic benefit.
Alternatives and complementary options
Non-surgical choices include topical minoxidil, oral 5-alpha-reductase inhibitors, prostaglandin analogs being investigated in trials, and cosmetic options such as scalp micropigmentation or concealers. For extensive diffuse thinning, hair systems or future regenerative therapies may be considered. For best-practice guidance on indications and safety, professional society materials can be consulted: International Society of Hair Restoration Surgery (ISHRS).
Practical tips to maximize long-term success
- Confirm candidacy with scalp mapping and donor density measurements before surgery.
- Combine surgery with proven medical therapy when genetic hair loss is ongoing.
- Follow postoperative care closely: avoid smoking, protect grafts from trauma, and follow physician timelines for washing and activity.
- Plan for staged procedures if large-area coverage or high density is desired; avoid unrealistic single-session promises.
Core cluster questions
- How long do transplanted hairs last compared with native hair?
- Who should avoid hair transplant surgery?
- What is the typical recovery and timeline after a hair transplant?
- How many grafts are needed for common balding patterns?
- What non-surgical options help preserve native hair before considering surgery?
Trade-offs when deciding on surgery
Trade-offs include cost versus benefit, the potential need for multiple procedures, and the balance between scar visibility (FUT) and graft yield (FUE). FUT can yield more grafts per session but leaves a linear scar; FUE leaves tiny punctate scars with slower aggregate harvest in some patients. Surgical choice depends on future plans, scalp laxity, and lifestyle considerations.
When a hair transplant is not a cure
Hair transplant is not a pharmaceutical cure that halts the underlying biological process of androgenetic alopecia across the entire scalp. If the native follicles continue to miniaturize, the overall hairline and density will change over time. Managing expectations and planning maintenance strategies turns a one-time procedure into a long-term plan for hair health.
Final checklist before booking a procedure
- Verify credentials and membership in recognized societies (e.g., ISHRS).
- Request photographic examples of results for similar patient types.
- Receive a written plan with graft counts, expected density, and staged options.
- Discuss medical therapy integration and long-term maintenance costs.
FAQ
Does hair transplant cure baldness permanently?
Transplanted follicles usually survive long-term, so the grafts themselves are often permanent. However, the procedure does not cure the underlying tendency to lose native hair, so ongoing hair loss can alter the overall appearance unless managed with medical therapy or future procedures.
How long until transplanted hair looks natural?
Initial growth commonly appears at 3–6 months; cosmetic improvement is visible by 6–9 months, and final maturation usually by 12–18 months when thickness and pattern settle.
What are the main differences between FUE and FUT?
FUE removes individual follicular units with small punches, leaving dot-like scars and faster healing. FUT removes a strip of scalp and harvests follicles from it, which can yield more grafts per session but leaves a linear scar. Choice depends on donor characteristics and patient goals.
Can medication stop the need for surgery?
Medications such as topical minoxidil and oral finasteride can slow or stabilize hair loss for many people and sometimes improve density, but they rarely restore a full head of hair in advanced cases. Medical therapy may reduce or delay the need for surgery and is often used alongside transplantation.
How much does a hair transplant cost and is it worth it?
Costs vary by region, technique, and graft number. Value depends on expectations, cosmetic goals, and long-term maintenance. A thorough consultation that evaluates donor supply, pattern, and ongoing treatments helps determine whether the expected outcome justifies the cost.