Depression Explained: Causes, Symptoms, and Effective Treatments
👉 Best IPTV Services 2026 – 10,000+ Channels, 4K Quality – Start Free Trial Now
Depression Causes, Symptoms, and Treatments
This guide outlines depression causes, symptoms, and treatments with clear definitions, practical assessment steps, and treatment options for people seeking reliable, evidence-based information.
- Depression is a common, diagnosable medical condition with biological, psychological, and social causes.
- Common symptoms include persistent low mood, loss of interest, changes in sleep or appetite, and cognitive changes.
- Effective treatments include psychotherapy, medication, lifestyle changes, and structured care plans; choice depends on severity and preference.
What is depression?
Depression is a clinical condition—often called major depressive disorder when criteria are met—characterized by persistent low mood, diminished interest in activities, and impaired daily functioning. Related terms include depressive episode, dysthymia (persistent depressive disorder), and seasonal affective disorder. Official diagnostic criteria are detailed by professional bodies such as the American Psychiatric Association and ICD-11.
Causes: why depression develops
Causes usually span biological, psychological, and social domains. Common contributors include genetics, brain chemistry (neurotransmitter and circuit-level differences), chronic medical conditions, trauma, stress, and social isolation. Medication effects, substance use, and certain endocrine disorders can also trigger depressive episodes.
Biological factors
Family history, inflammatory markers, hormonal changes, and brain network differences have recognized roles. Genetic vulnerability does not mean inevitability—environment interacts with biology.
Psychological and social factors
Cognitive patterns (like negative thinking), early adverse experiences, loss, unemployment, and relationship problems increase risk. Social determinants—housing, income, and support—are strong modifiers of course and recovery.
Recognizing symptoms and signs
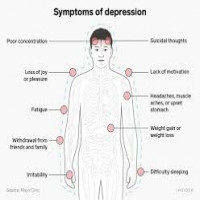
Key symptoms include prolonged sadness, reduced interest or pleasure, significant weight change, sleep disturbance, fatigue, slowed thinking or agitation, feelings of worthlessness or guilt, difficulty concentrating, and suicidal thoughts. Medical evaluation rules out other causes. Phrases readers search for include signs of major depressive disorder and how to recognize depression in adults.
Screening and diagnosis
Brief screening tools such as the PHQ-9 are widely used in primary care to measure symptom burden and guide next steps. Positive screens require clinical evaluation for diagnosis, risk assessment, and safety planning when suicide risk is present.
Treatment options for depression
Treatment selection depends on severity, prior treatment response, comorbid conditions, and personal preferences. Typical options include psychotherapy, antidepressant medication, combined approaches, and structured lifestyle interventions. For treatment-resistant cases, other modalities—like electroconvulsive therapy (ECT), transcranial magnetic stimulation (TMS), or specialist care—may be considered.
Psychotherapy
Evidence-based psychotherapies include cognitive behavioral therapy (CBT), interpersonal therapy (IPT), and behavioral activation. These address negative thinking patterns, interpersonal problems, and activity scheduling to restore function.
Medication
Antidepressants (SSRI, SNRI, atypical agents) can reduce symptoms and lower relapse risk. Medication choice balances side effects, medical interactions, and patient preference. Regular follow-up and dose adjustments are standard practice.
Practical framework: the BIOPSYCH-SOCIAL Checklist
A structured checklist helps organize assessment and care planning. Use the BIOPSYCH-SOCIAL Checklist:
- Biological: medical history, medications, sleep, appetite, substance use, family history.
- Injury/Illness: recent physical illness, endocrine issues, pain.
- Obvious risks: suicidal ideation, self-harm, access to means.
- Psychological: mood symptoms, cognition, trauma history.
- Social: housing, employment, relationships, support network.
- Yield to severity: determine level of care (outpatient vs urgent).
- Care plan: psychotherapy, medication, follow-up schedule, crisis plan.
Short real-world example
Scenario: A 35-year-old experiences low mood for two months, losing interest in hobbies and sleeping poorly. A primary care clinician administers a PHQ-9, reviews medications, rules out thyroid disease, and discusses CBT referral plus a short trial of an SSRI. A safety plan and follow-up at two weeks are scheduled; outcomes are tracked with follow-up PHQ-9 scores.
Practical tips
- Get a medical check: rule out reversible causes (thyroid, B12, medications).
- Use a validated screening tool (PHQ-9) to track symptoms over time.
- Ask about safety: directly ask about suicidal thoughts and create a documented safety plan if needed.
- Combine treatments: psychotherapy plus medication often works better than either alone for moderate to severe depression.
- Monitor and adjust: allow 4–8 weeks to assess antidepressant response and adjust therapy based on measurable outcomes.
Common mistakes and trade-offs
Common mistakes include assuming a single cause, underestimating social factors, and discontinuing medication too early. Trade-offs often involve balancing speed of symptom relief with side effects—medication can act faster for severe symptoms, while therapy builds skills for long-term relapse prevention. For some, immediate medication is appropriate; for others, starting with therapy or lifestyle changes may be preferred.
Reliable resources and next steps
For prevalence, diagnostic criteria, and global guidance, consult the World Health Organization's fact sheet on depression (WHO). Local primary care, mental health clinics, and licensed therapists are appropriate next contacts. If immediate danger exists, use emergency services or crisis lines.
Core cluster questions for further reading
- What triggers depression in adults?
- How is depression diagnosed in primary care?
- What are evidence-based treatment plans for moderate depression?
- How to manage antidepressant side effects and when to change medication?
- What support helps prevent relapse after recovery from depression?
FAQ
What are the most common depression causes, symptoms, and treatments?
Common causes include genetic vulnerability, life stressors, medical conditions, and substance use. Typical symptoms are persistent low mood, loss of interest, sleep and appetite changes, and concentration problems. Treatments range from psychotherapy and antidepressants to combined care and, in severe or resistant cases, specialist interventions like ECT or TMS.
How quickly do antidepressants work?
Antidepressants often begin to show effects within 2–4 weeks, with fuller benefit by 6–8 weeks. Close follow-up is important to assess response and side effects.
Can lifestyle changes help with depression?
Yes. Regular exercise, structured sleep, reduced alcohol use, and social support can reduce symptoms and improve treatment response when used alongside therapy or medication as indicated.
How to recognize signs of major depressive disorder?
Key signs include persistent depressed mood or loss of interest for two weeks or longer, plus at least four additional symptoms such as major sleep or appetite change, fatigue, difficulty concentrating, feelings of worthlessness, or suicidal thoughts. Professional assessment is required for diagnosis.
When should a person seek urgent help?
Seek immediate help if there are suicidal thoughts, plans, intent, or if self-care ability is dangerously impaired. Emergency services, crisis hotlines, or urgent psychiatric care are appropriate in such situations.