Microneedling Treatment: Benefits, Safety, and Practical How-To Guide
Get a free topical map and start building content authority today.
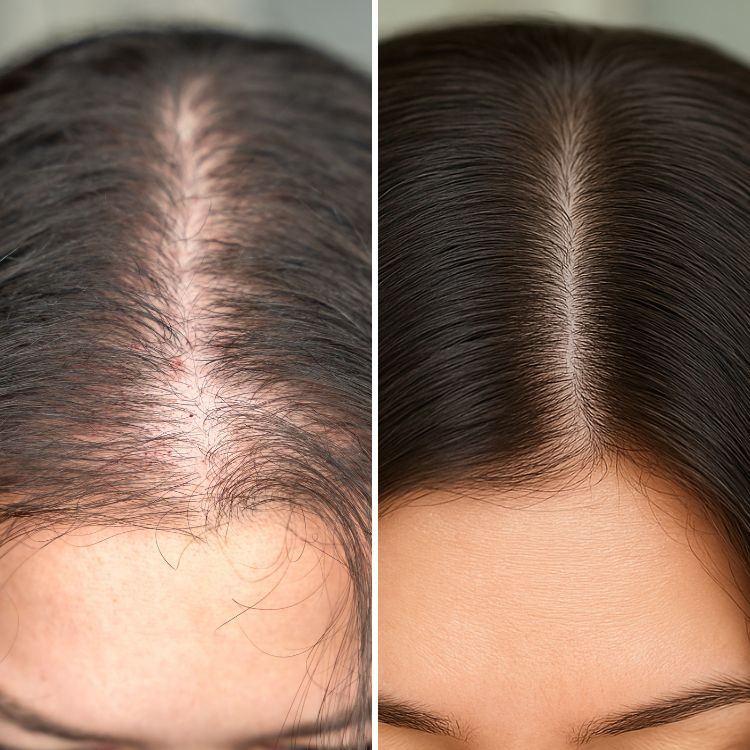
Microneedling treatment offers a practical way to improve skin texture, reduce scarring, and stimulate collagen production. This guide explains what microneedling is, who is a suitable candidate, the differences between professional and at-home approaches, and clear steps to prepare, perform, and recover from a session.
- Microneedling (collagen induction therapy) uses controlled micro-injuries to trigger skin repair.
- Professional treatments are safer and more effective for deep scars or advanced concerns; at-home devices suit mild texture work if used correctly.
- Key steps: medical review, device selection, clean technique, planned downtime, and outcome tracking.
Detected intent: Informational
What is microneedling treatment?
Microneedling treatment, also called collagen induction therapy, involves using fine needles to create controlled microchannels in the epidermis. These micro-injuries stimulate the skin's natural repair mechanisms, increasing collagen and elastin production. Devices vary from manual dermarollers to automated pen systems and professional clinic devices, including radiofrequency-assisted needles (RF microneedling).
How microneedling works and what it treats
At a biological level, micro-injury triggers a cascade: platelet activation, growth factor release, and fibroblast-mediated collagen synthesis. Clinically, microneedling is used for acne scars, surgical scars, enlarged pores, fine lines, uneven texture, and some types of hyperpigmentation when combined with appropriate topical agents. For certain conditions, combinations such as PRP (platelet-rich plasma) or topical vitamin C can be used to enhance results.
Related terms and technologies
Common related terms include dermaroller, dermapen, percutaneous collagen induction, RF microneedling, platelet-rich plasma (PRP), epidermal remodeling, and transepidermal delivery.
Medical microneedling benefits vs at-home microneedling safety
Understand the trade-offs between professional and DIY options. Professional medical microneedling benefits include deeper penetration, sterilized conditions, pain management, and tailored protocols for specific scar depths or pigment issues. At-home microneedling safety is acceptable only for short needles and strict hygiene; it should not be used for active acne, suspicious lesions, or deep scar remodeling.
Trade-offs and common mistakes
Common mistakes include using too-long needles at home, skipping antiseptic technique, treating active infections, and applying inappropriate topical agents immediately after treatment (which can increase irritation or risk). Trade-offs: deeper needling delivers stronger collagen stimulation but increases downtime, bruising, and infection risk. Superficial at-home needling has less downtime but also more limited effects.
MICRO checklist: a practical framework to plan a microneedling session
Use the MICRO checklist to prepare and follow up on treatments:
- Medical review — check history, medications, and skin conditions.
- Instrument selection — choose device and needle depth appropriate for concern.
- Clean technique — strict sanitation, single-use tips, and sterile environment.
- Recovery plan — pain control, wound care, sunscreen, and activity restrictions.
- Outcomes tracking — photos, symptom log, and timeline for follow-up.
Step-by-step: what to expect before, during, and after a session
Before the session
Stop retinoids and exfoliating acids 3–7 days before a professional session. Disclose medications like isotretinoin, which often requires delaying invasive procedures. Schedule a consultation to set realistic goals and plan topical adjuncts.
During the session
Professional sessions use topical numbing, sterile single-use tips, and controlled needle depths. Sessions typically last 20–60 minutes depending on area. At-home devices require gentler pressure, short needle lengths (generally <0.5 mm), and careful hygiene.
Aftercare and recovery
Expect redness and mild swelling for 24–72 hours. Use gentle cleansers, moisturizers, and daily broad-spectrum sunscreen. Avoid aggressive exfoliants, heat exposure, and direct sun until fully healed.
Practical tips for better results
- Choose a trained provider or, for home use, follow device instructions and favor single-use sterile tips.
- Avoid microneedling over active acne, open wounds, or suspicious pigmented lesions.
- Use sun protection diligently for at least two weeks post-procedure to reduce hyperpigmentation risk.
- Space sessions according to needle depth: 4–6 weeks for deeper clinic treatments, and longer intervals for aggressive protocols.
Real-world example: a typical acne-scar plan
Scenario: A 32-year-old with rolling acne scars seeks improvement. Plan: three professional microneedling sessions spaced six weeks apart using a device set to appropriate depths for scar remodeling, combined with topical LED therapy post-treatment and strict SPF afterward. Photos at baseline and after each session track progress. Improvement usually appears after the second session and continues for months as collagen matures.
Core cluster questions for internal linking
- How does microneedling compare with laser resurfacing for scar treatment?
- What is the typical recovery timeline after a professional microneedling session?
- Which skin types respond best to microneedling for hyperpigmentation?
- Can microneedling enhance topical product absorption and which serums are safe to use?
- What are the contraindications for microneedling and when to consult a dermatologist?
Safety, standards, and where to learn more
Follow guidance from dermatology organizations and device manufacturers. For authoritative patient-facing recommendations about safety and who should consult a dermatologist, see the American Academy of Dermatology: American Academy of Dermatology.
Common mistakes to avoid
- Using unsterilized or shared rollers/pens — infection risk is real.
- Expecting dramatic results after a single mild session — collagen remodeling takes months and multiple treatments.
- Applying irritating actives immediately after needling without professional guidance.
When to seek professional care
Seek a dermatologist if there is excessive bleeding, signs of infection (increasing pain, spreading redness, pus), or unusual pigment changes after treatment. Also consult a licensed clinician when treating complex scarring, keloid-prone skin, or when on systemic medications like isotretinoin.
Practical takeaway
Microneedling treatment is a well-established method for stimulating collagen and improving skin texture when performed with proper planning, infection control, and aftercare. Use the MICRO checklist to prepare, choose the appropriate setting for the concern, and track outcomes with photos and scheduled follow-ups.
FAQ: What is microneedling treatment?
Microneedling treatment creates controlled micro-injuries to stimulate natural collagen production, useful for acne scars, fine lines, and texture concerns. Professional treatments offer deeper and safer results for significant scarring while at-home devices may help with mild texture improvement when used correctly.
How safe is at-home microneedling safety?
At-home devices can be safe for short-needle, low-intensity use when single-use sterile tips and strict hygiene are followed. Avoid deep needling at home and do not treat active skin infections or open wounds.
How many sessions are needed for visible improvement?
Visible improvement commonly requires 3–6 sessions spaced 4–8 weeks apart, depending on the depth of concerns and the device used. Collagen remodeling continues for months after treatment.
Can microneedling be combined with other treatments?
Yes. Microneedling is often combined with PRP, topical growth factors, or light-based therapies to enhance results, but combinations should be chosen based on skin type and clinical goals by a qualified clinician.
Are there any long-term risks?
Long-term risks are low when treatments follow clinical standards. Improper technique, poor hygiene, or treating inappropriate conditions can lead to infection, scarring, or pigment changes. Consult a dermatologist for individualized risk assessment.