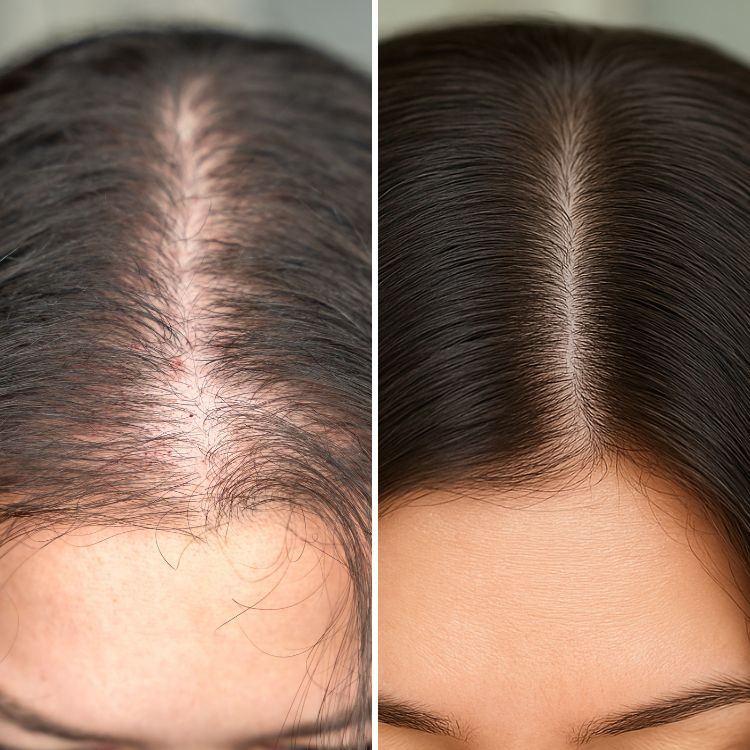
FUE Hair Transplant Guide: Procedure, Recovery, and What to Expect
Get a free topical map and start building content authority today.
FUE hair transplant is a widely used surgical method for restoring hair by extracting individual follicular units from a donor area and implanting them into thinning or balding scalp sites. The technique, known as follicular unit extraction, is one of the main approaches to hair restoration and is discussed here in terms of process, candidacy, expected outcomes, and common risks.
- FUE (follicular unit extraction) removes single hair grafts from a donor area for transplanting into thinning regions.
- Typical recovery is days to weeks for initial healing and several months for regrowth; final results may take 9–12 months.
- Not all candidates are suitable; candidacy depends on donor supply, hair characteristics, and scalp health.
- Potential risks include scarring, infection, shock loss, and variable graft survival; discuss regulatory standards and credentials when choosing a clinic.
Understanding FUE hair transplant
FUE hair transplant refers to a minimally invasive method in which clinicians harvest individual follicular units—typically one to four hairs each—from a donor area, often the back or sides of the scalp. Those grafts are then implanted into recipient sites designed to mimic natural hair direction and density. Terms commonly associated with the procedure include grafts, donor strip (in contrast with strip harvesting methods), micrografting, follicular anatomy, and recipient site creation.
How the procedure works
Extraction
Extraction uses a small, circular punch (manual or motorized) to free follicular units from surrounding tissue. The size of the punch and extraction technique affect wound size and likelihood of visible scarring. Extracted grafts are stored in a preservation solution until implantation.
Recipient site creation and implantation
Small incisions or slits are made in the recipient area to receive grafts. Implantation aims to reproduce natural hair angle and density. Implant techniques vary—some practitioners use forceps or implanter pens—to optimize placement and graft survival.
Duration and anesthesia
Procedures typically take several hours to a full day depending on graft count. Local anesthesia is commonly used to numb the scalp during treatment.
Who may be a candidate
Good candidates usually have sufficient donor hair resistant to androgenetic hair loss and realistic expectations about achievable density. Factors evaluated include pattern and progression of hair loss, donor area quality, age, scalp laxity, and overall health. Conditions that can affect candidacy include active scalp disease, certain systemic illnesses, or insufficient donor supply.
Recovery, timeline, and expected results
Immediate recovery
After a session, mild swelling, redness, and scabbing in donor and recipient areas are common. Bandaging may be minimal. Pain is generally controlled with over-the-counter analgesics or prescription medication when indicated.
Short-term timeline
Grafts typically settle within a few days. Many patients experience 'shock loss'—temporary shedding of transplanted or native hairs—which is usually transient.
Long-term regrowth
Visible regrowth often begins around three to four months post-procedure, with continued improvement up to 9–12 months. Final density depends on graft survival, native hair characteristics, and whether additional sessions are performed.
Risks, complications, and how outcomes are measured
Common risks include infection, folliculitis, scarring (including small circular scars at extraction sites), poor graft survival, and unnatural hairline design if placement is not skillful. Outcomes are typically measured by graft survival rates, aesthetic integration, and patient satisfaction. Clinical societies such as the International Society of Hair Restoration Surgery (ISHRS) provide practice guidelines and data summaries that can help contextualize expected results.
Cost, regulation, and choosing a provider
Costs vary widely by geographic region, number of grafts, and practitioner expertise. Regulatory oversight differs by country: in the United States, facilities and clinicians may be accredited by medical boards and guidelines exist from specialty organizations; national health services and regulatory agencies publish consumer information about licensed practitioners. When evaluating providers, consider clinician qualifications (e.g., board certification in dermatology or plastic surgery), clinic accreditation, before-and-after documentation, and transparent reporting of risks and costs.
For authoritative consumer guidance on hair loss and treatment options, refer to resources from established health organizations such as the NHS on hair loss and treatments: NHS — Hair loss.
Alternatives and complementary approaches
Non-surgical options can include topical treatments, prescription medications, cosmetic concealers, and platelet-rich plasma (PRP) therapies; these may be used alone or as adjuncts to surgical restoration. Choice of treatment depends on diagnosis, severity, and patient goals.
Preparing for a consultation
During an initial assessment, expect evaluation of hair loss pattern, donor availability, medical history, and photographic documentation. A proposed treatment plan should outline graft numbers, anticipated outcomes, risks, recovery expectations, and cost estimates. Credentials, facility standards, and infection control practices are relevant topics for discussion.
Long-term considerations
Hair loss can be progressive; maintaining realistic expectations about density and the potential need for future procedures is important. Long-term results depend on the stability of the donor supply and ongoing care of scalp and hair health.
Frequently asked questions
What is an FUE hair transplant and how does it differ from other methods?
FUE (follicular unit extraction) involves harvesting individual follicular units, whereas strip methods remove a linear strip of scalp (follicular unit transplantation, FUT). FUE typically results in smaller, scattered scalp scars and may allow quicker recovery, while FUT can yield a larger number of grafts in a single session with a linear scar at the donor site.
How long does it take to see results after an FUE hair transplant?
Hair growth usually begins around three to four months, with progressive improvement up to 9–12 months; complete maturation of grafts and final cosmetic outcome may take up to a year or longer.
What are common complications following FUE hair transplant?
Potential complications include minor bleeding, infection, folliculitis, small scars at extraction sites, shock loss of native hairs, and variable graft survival leading to less-than-expected density. Clinic protocols for sterile technique and postoperative care aim to minimize these risks.
Is an FUE hair transplant suitable for everyone?
Not all individuals are suitable candidates. Adequate donor supply, realistic expectations, and absence of contraindicating scalp or systemic conditions are important. Assessment by a qualified clinician helps determine suitability based on individual factors.
How should results of an FUE hair transplant be evaluated?
Evaluation includes photographic documentation, assessment of graft survival and coverage, naturalness of hairline and angulation, and patient satisfaction. Follow-up appointments allow monitoring of healing and regrowth progress.