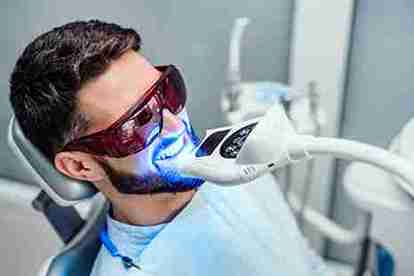
How Laser Treatments Affect Underarm Skin Tone: Risks, Results, and Aftercare
FREE SEO Topical Map Generator: Find Your Next Content Ideas
Detected intent: Informational
The phrase "laser underarm skin tone" reflects a common concern: how laser procedures — especially laser hair removal — change the color or texture of the skin under the arm. This article explains mechanisms, likely outcomes, safe practices, and realistic expectations so readers can decide whether a laser treatment is appropriate for underarm skin.
- Lasers can lighten, darken, or rarely cause textural change in underarm skin via targeted melanin disruption or post-inflammatory reactions.
- Risk depends on skin tone, laser type, treatment settings, and pre/post care. Consultation with a qualified clinician reduces complications.
- Follow the LASER-SAFE checklist and 3–5 practical tips in this guide for safer, better results.
Laser underarm skin tone: how lasers affect underarm pigmentation
Lasers interact with melanin and blood vessels. In the underarm area, two main outcomes are most relevant: reduction of pigment (lightening) when melanin is selectively destroyed and removal of hair follicles, or increased pigmentation (darkening) through post-inflammatory hyperpigmentation (PIH) or thermal injury. The risk profile is shaped by baseline skin tone, choice of device (Nd:YAG, diode, alexandrite, fractional lasers), and technique.
Key mechanisms: why color changes happen
Melanin absorption and selective photothermolysis
Lasers target melanin in the hair shaft and follicle. The absorbed energy converts to heat and damages the follicle. If surrounding epidermal melanin absorbs excess energy — common in darker skin tones — the epidermis can sustain thermal stress, producing hypopigmentation (lighter patches) or hyperpigmentation (darker patches).
Post-inflammatory hyperpigmentation (PIH)
Any skin injury or irritation — including burns, aggressive laser pulses, or strong topical peel agents used at the same time — can trigger inflammation. Inflammation signals melanocytes to produce more melanin, causing PIH. PIH can appear days to weeks after treatment and may persist for months without appropriate care.
Textural changes and scarring
Excessive energy settings, overlapping pulses, or inexperienced technique can produce superficial or deeper injury, potentially causing scarring or altered skin texture in the underarm valley. Scarring is uncommon with modern devices when used correctly but remains a possible trade-off.
Who is at higher risk?
Risk factors for unwanted changes in underarm skin tone include darker Fitzpatrick skin types (IV–VI), recent tanning, history of PIH, active inflammatory skin conditions (eczema, folliculitis), or use of photosensitizing medications. A patch test, conservative settings, and devices suited to higher melanin levels (for example, Nd:YAG lasers at longer wavelengths) lower the risk.
LASER-SAFE checklist (named framework)
Use this 6-step LASER-SAFE checklist before and after treatment to reduce complications:
- Look for qualified practitioner (board-certified dermatologist/plastic surgeon or certified laser technician under medical oversight).
- Assess skin type and history (Fitzpatrick type, PIH history, recent tanning).
- Select appropriate device and settings for underarm skin and hair density.
- Execute a patch test on a small underarm area and wait 2–4 weeks for reaction.
- Review pre- and post-care instructions (sun avoidance, topical steroid if needed, gentle cleansing).
- Schedule follow-ups to monitor pigmentation and manage complications early.
Practical tips for safer results
- Avoid tanning for 4–6 weeks before and after treatment; increased epidermal melanin raises PIH risk.
- Request a conservative, low-fluence test spot first; evaluate color change only after 2–4 weeks.
- Use gentle anti-inflammatory aftercare (cool compresses, fragrance-free emollients) and avoid harsh peels or scrubs on treated skin.
- If darkening occurs, early treatment with topical agents (e.g., sunscreen, azelaic acid, or prescribed hydroquinone under clinician supervision) and sun avoidance speeds resolution.
- Discuss laser type; longer wavelengths (1064 nm Nd:YAG) penetrate deeper and are often safer on darker skin for hair removal than shorter-wavelength devices.
Common mistakes and trade-offs
Common mistakes
- Choosing high-fluence settings to speed results — increases risk of thermal injury and PIH.
- Skipping a patch test, especially in darker skin tones or after tanning.
- Combining aggressive chemical exfoliation or topical bleaching agents immediately before or after laser without guidance.
Trade-offs
Faster hair reduction often requires higher energy and more aggressive settings, which increase pigment risk. Choosing gentler settings may require more sessions but reduces chance of permanent color change. Device selection also involves trade-offs: alexandrite and diode lasers are efficient for lighter skin, while Nd:YAG is safer for darker skin but may be slightly less comfortable or require more sessions.
Real-world example
A 30-year-old with Fitzpatrick type IV sought underarm laser hair removal. The clinician performed a patch test using a Nd:YAG device at conservative settings. Mild redness but no darkening occurred after 3 weeks; sessions proceeded with incremental energy increases. After five sessions and strict sun protection, hair density dropped by 70% and no PIH developed. This scenario demonstrates risk mitigation through device choice, patch testing, and conservative, staged treatment.
When to seek medical help
Contact a clinician if the underarm develops worsening pain, blistering, spreading dark patches, or signs of infection. Early treatment of burns and inflammatory hyperpigmentation improves outcomes. For guidance on laser hair removal safety, review resources from professional dermatology organizations.
Authoritative guidance: American Academy of Dermatology: Laser hair removal
Core cluster questions
- How long does underarm discoloration after laser usually last?
- Which laser types are safest for darker underarm skin?
- What pre-treatment steps reduce the risk of post-inflammatory hyperpigmentation?
- Can topical products correct darkening caused by laser treatments?
- How many laser sessions are typically needed to avoid repeated irritation of the underarm?
Practical takeaways
- Evaluate provider qualifications and request a patch test when concerned about underarm pigment changes.
- Prefer longer wavelengths and conservative settings for darker skin tones.
- Follow aftercare: sun avoidance, gentle skincare, and early medical review for unexpected darkening or burns.
FAQ
Will laser underarm skin tone always get lighter after treatment?
No. Outcomes vary. Some people experience lightening if melanin in hair follicles is reduced, while others experience darkening due to PIH or superficial burns. Results depend on skin tone, laser type, and practitioner technique.
Can laser hair removal cause permanent dark underarm discoloration?
Permanent darkening is uncommon when treatment is performed correctly but can occur after deep thermal injury or repeated inflammation. Early management of PIH and appropriate device selection reduce long-term risk.
What is the best way to prevent underarm hyperpigmentation after laser?
Preventive steps include avoiding tanning, scheduling a patch test, using conservative energy settings, employing gentle post-treatment care, and protecting the area from UV exposure immediately after treatment.
How soon should a patch test be checked for pigment changes?
A patch test should be evaluated at 2–4 weeks. This timeframe allows delayed PIH to appear and gives a useful preview of how the skin responds before treating larger areas.
Can topical creams fix underarm hyperpigmentation after laser?
Topical agents like azelaic acid, niacinamide, or prescription-strength hydroquinone (under clinician supervision) can lighten PIH. Sun protection and anti-inflammatory care are essential alongside topical treatment. Severe or resistant cases may require in-office procedures performed by a dermatologist.