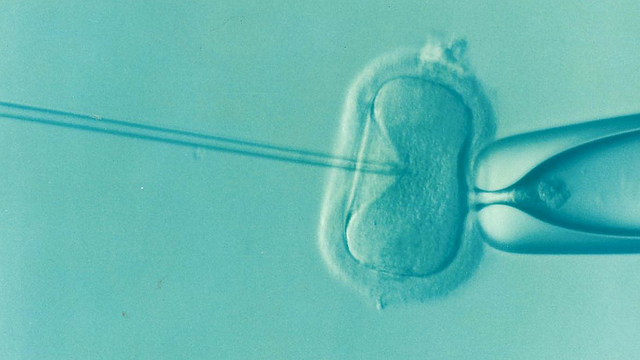
What Diminished Ovarian Reserve Really Means for Your Fertility Treatment
FREE SEO Topical Map Generator: Find Your Next Content Ideas
Few fertility test results carry the emotional weight of a low AMH. Anti-Müllerian hormone is a protein produced by the small follicles in your ovaries, and its level in the blood provides one of the most reliable available estimates of how many eggs remain in your ovarian reserve. When that number comes back lower than expected, particularly in a younger woman who did not anticipate any fertility challenges, the response is often a mixture of shock, grief, and urgent, anxious questions about what it means for the future.
What does a low AMH actually mean? Does it mean IVF will not work? Does it mean there is no time to lose? Does it mean donor eggs are inevitable? The answers to these questions are more nuanced and more hopeful than most patients initially expect, and understanding them clearly is the first and most important step toward making informed decisions about your treatment.
What AMH Actually Measures
AMH is produced by the granulosa cells surrounding the small antral follicles in your ovaries. Because its production is relatively constant throughout the menstrual cycle, it can be measured on any day and provides a stable snapshot of your current ovarian reserve. Higher AMH levels indicate a larger pool of resting follicles available for recruitment. Lower levels indicate a smaller pool.
What AMH does not measure is egg quality. This is one of the most important and most frequently misunderstood distinctions in fertility medicine. A woman with a low AMH may have a small number of eggs remaining, but those eggs can still be of good quality, particularly in younger women. Egg quality is primarily determined by age rather than ovarian reserve, which is why a 30-year-old woman with a low AMH has a meaningfully better prognosis than a 40-year-old with the same AMH level.
AMH is best understood as one piece of a larger diagnostic picture that also includes antral follicle count on transvaginal ultrasound, FSH levels, and the clinical context of the patient's age and reproductive history. No single test result should be used in isolation to draw conclusions about fertility potential or IVF outcomes.
What Low AMH Means for IVF
The primary clinical implication of a low AMH in the context of IVF is a reduced expected response to ovarian stimulation. Women with lower ovarian reserve typically produce fewer follicles and retrieve fewer eggs during a stimulation cycle than women with normal or high reserve. Fewer eggs mean fewer embryos, and fewer embryos reduce the number of opportunities available for transfer and the cumulative probability of success across multiple attempts.
This does not mean that IVF will not work. Many women with low AMH undergo IVF, retrieve a small number of eggs, and achieve successful pregnancies, sometimes on their first attempt. What low AMH does mean is that the process may require more cycles to accumulate sufficient embryos, that every retrieved egg carries additional significance, and that the treatment approach requires careful, individualised protocol design to maximise the response within the constraints of what the ovaries can produce.
The relationship between AMH and live birth rates in IVF is real but not deterministic. Studies consistently show that while poor responders have lower live birth rates per cycle than normal responders, many do achieve successful pregnancies, and cumulative success rates across multiple cycles are meaningfully higher than single-cycle rates suggest.
Protocol Strategies for Low AMH Patients
One of the most important decisions in managing low AMH in IVF is selecting the most appropriate stimulation protocol. The goal is to recruit as many of the available follicles as possible without over-suppressing the ovarian response or using a protocol that is poorly matched to the individual's reserve profile.
Several protocol approaches have been studied specifically in poor responder populations. The antagonist protocol is widely used because it avoids the prolonged suppression associated with long agonist protocols, which can further reduce the response in women with already limited reserve. Starting gonadotropin doses tend to be higher in low AMH patients to maximise follicle recruitment, though there is a ceiling beyond which additional medication produces diminishing returns.
Growth hormone supplementation has been studied as an adjuvant therapy in poor responders, with some evidence suggesting improved oocyte yield and embryo quality in selected patients. Testosterone priming, typically administered through transdermal gel in the weeks before stimulation, has also shown promise in improving ovarian response in women with diminished reserve by increasing androgen levels in the follicular environment in a way that sensitises follicles to FSH stimulation.
The POSEIDON classification system, developed specifically to categorise and guide treatment for patients with poor ovarian response, has provided a useful framework for individualising protocol decisions based on age, AMH, antral follicle count, and previous stimulation history. Clinicians familiar with this system can design more precisely targeted approaches for low AMH patients than a generic poor responder protocol allows.
The Egg Banking Strategy
For women with very low AMH where a single stimulation cycle is likely to yield only one or two eggs, an egg or embryo banking strategy may be the most clinically appropriate approach. This involves conducting multiple consecutive retrieval cycles with the goal of accumulating a sufficient number of eggs or embryos before proceeding to transfer.
Banking allows the cumulative embryo pool from several cycles to be assessed together, giving the medical team the best possible selection of embryos for transfer and genetic testing if applicable. It requires patience and emotional resilience because it delays the transfer phase of treatment, but it significantly improves the overall probability of a successful pregnancy compared to proceeding to transfer after each individual retrieval regardless of how few embryos result.
Preimplantation genetic testing can be incorporated into a banking strategy for older low AMH patients where the risk of chromosomal abnormality in embryos is elevated. Testing identifies which banked embryos are chromosomally normal before transfer, ensuring that the limited embryos available are used as effectively as possible.
Lifestyle and Supplementation Strategies for Low AMH
While AMH itself cannot be significantly increased through lifestyle interventions, the quality of the eggs that remain in a diminished ovarian reserve can be supported through targeted nutritional and lifestyle strategies.
CoQ10 is the most widely studied and most consistently recommended supplement for women with low AMH. Its role in supporting mitochondrial energy production within developing egg cells is directly relevant to egg quality, and doses of 400 to 600 mg daily in the months before an IVF cycle are commonly recommended by fertility specialists working with poor responder patients. The evidence base for CoQ10 in this population is among the strongest of any nutritional supplement studied in reproductive medicine.
DHEA supplementation has been used in poor responder IVF protocols for over a decade, with some evidence suggesting improvements in ovarian response, egg quality, and pregnancy rates in selected patients. It is not appropriate for all women and requires specialist guidance before use, but it represents a potentially meaningful adjunct for appropriately selected low AMH patients.
Vitamin D, omega-3 fatty acids, melatonin, and a high-quality prenatal multivitamin all contribute to the nutritional environment in which your remaining follicles develop. Avoiding smoking, limiting alcohol, managing stress, and maintaining a healthy body weight are lifestyle factors that support the best possible egg quality from whatever reserve remains.
Connecting with a knowledgeable best ivf center in jaipur that has specific experience managing poor responder patients ensures that your protocol is designed with genuine expertise in maximising outcomes from a limited ovarian reserve, and that supplementation and lifestyle recommendations are personalised to your specific diagnostic profile.
When Donor Eggs Become Part of the Conversation
For some women with very low AMH, particularly those who are older or who have had multiple unsuccessful IVF cycles with poor response, donor egg IVF eventually becomes part of the clinical conversation. This is not a failure. It is a pathway to parenthood that carries significantly higher success rates than own-egg IVF in women with severely diminished reserve, and it is one that many couples find deeply fulfilling.
The decision to pursue donor eggs is a deeply personal one that deserves time, reflection, and appropriate counselling support. Most women benefit from exploring all available options with their own eggs before making this decision, and a good fertility specialist will support that process without rushing toward donor eggs prematurely or avoiding the conversation when it genuinely becomes clinically appropriate.
For comprehensive guidance on all available pathways whether pursuing own-egg IVF with an optimised protocol or exploring donor egg options, a trusted test tube baby center in jaipur with experienced reproductive specialists and a compassionate, patient-centred approach gives you the honest, personalised counsel you need to make the decisions that are right for your individual situation.
Final Thoughts
A low AMH is not a full stop. It is a clinical data point that changes some aspects of your treatment planning but does not eliminate the possibility of success. Many women with diminished ovarian reserve have built their families through IVF, and the advances in protocol design, supplementation strategies, and embryo banking techniques available today give poor responder patients better options than at any previous point in reproductive medicine.
Know your numbers. Understand what they mean and what they do not mean. Work with a team that specialises in your situation. And do not let a single test result define the limits of what is possible for you.