Microneedling Guide for Skin Rejuvenation: Benefits, Risks, and Aftercare
Introduction
Microneedling has gained attention as a minimally invasive option for skin rejuvenation that stimulates collagen production and can improve texture, fine lines, and some types of scarring. This article summarizes how microneedling works, potential benefits, common risks and contraindications, and practical guidance on preparation and aftercare. Information is intended for general knowledge and not a substitute for professional medical advice.
- Microneedling creates controlled micro-injuries to trigger collagen and elastin remodeling.
- It may improve skin texture, reduce fine lines, and help some types of acne scarring.
- Risks include temporary redness, infection, scarring, and pigment changes; results vary by skin type and technique.
- Choosing a licensed practitioner and following aftercare reduces complications.
Microneedling: What it is
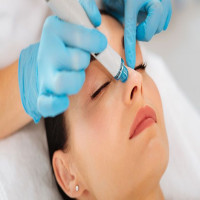
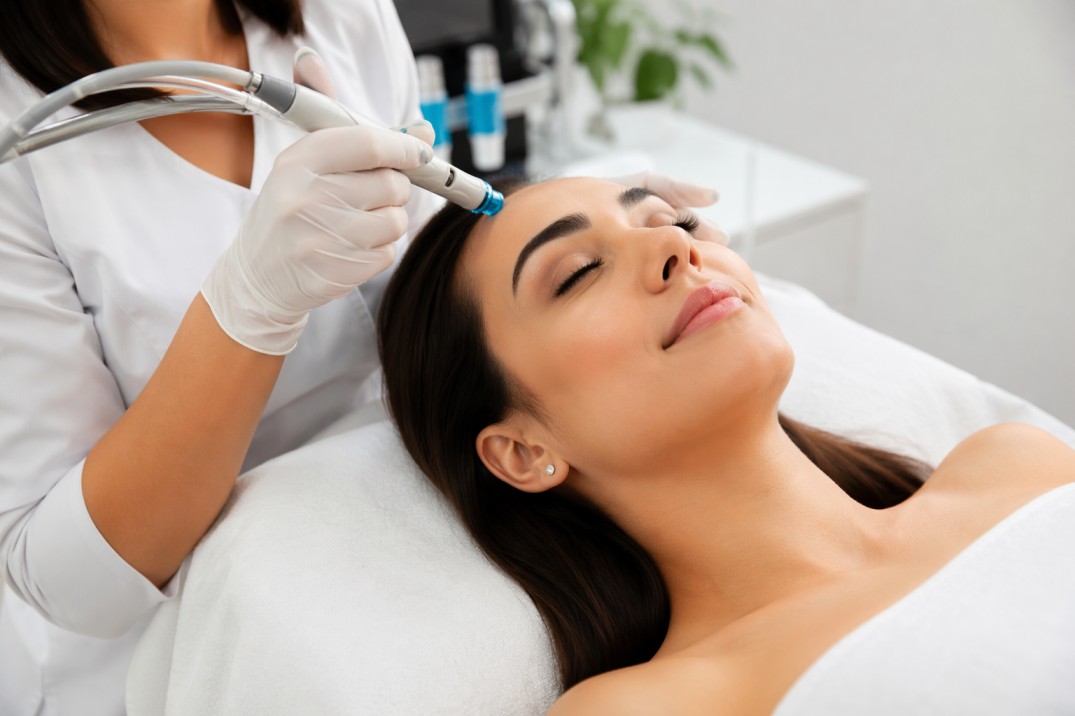
Microneedling, also described as collagen induction therapy, uses small sterile needles to create microchannels in the epidermis and superficial dermis. Devices range from manual rollers (dermarollers) to motorized pens with adjustable needle depths. The controlled injury causes a wound-healing response that can increase collagen and elastin synthesis and enhance absorption of topical serums applied during or after treatment.
How microneedling works
Mechanism
The micro-injuries produced by needles initiate a cascade of wound-healing processes: platelet activation, release of growth factors, and fibroblast stimulation. Over weeks to months these processes can remodel dermal collagen and improve skin firmness and texture. Needle depth, treatment frequency, and device type influence depth of effect.
Adjuncts and variations
Microneedling is sometimes combined with topical agents such as hyaluronic acid, vitamin serums, or platelet-rich plasma (PRP) to potentially enhance outcomes. Evidence quality varies by adjunct; some clinical studies reported improved scarring and pigmentation with combined protocols, but results depend on technique and patient selection.
Potential benefits
- Improvement in skin texture and firmness
- Reduction of fine lines and superficial wrinkles
- Reduction in some types of acne scarring and stretch marks
- Enhanced penetration of topical treatments
Risks, side effects, and contraindications
Common short-term effects
Temporary redness, mild swelling, pinpoint bleeding, and sensitivity are common and typically resolve within days. Downtime varies by needle depth and individual healing.
Less common but serious risks
Infection, prolonged redness, scarring, and post-inflammatory hyperpigmentation can occur, particularly when performed improperly or on unsuitable skin types. People with active acne, eczema, psoriasis, keloid tendency, or certain blood-clotting disorders may be advised against treatment. Use of isotretinoin within prior months is often a contraindication. Consultation with a licensed dermatologist or qualified clinician is recommended to assess suitability.
Preparing for treatment
- Disclose medical history, medications, and recent procedures to the provider.
- Avoid sunburn, aggressive exfoliation, and certain topical medications (such as retinoids) before treatment per provider instructions.
- Confirm that sterile, single-use needles and appropriate infection-control measures will be used.
Aftercare and recovery
Immediate care
Expect redness and mild swelling. Follow provider guidance on cleansing and on which topical products to use. Avoid heavy makeup, direct sun exposure, and sweating for the initial healing period to reduce infection and pigment risk.
When to seek follow-up
Seek professional advice if signs of infection (increasing pain, pus, fever) occur, if there is unexpected prolonged bruising, or if pigment changes develop. Routine follow-up helps track progress and plan repeat sessions if appropriate.
Comparing microneedling with other resurfacing options
Compared with ablative laser resurfacing, microneedling generally has shorter downtime and lower risk of severe pigment changes, but may deliver more modest improvements per session. Chemical peels and non-ablative lasers are alternative or complementary options. Treatment choice should consider skin type, target concerns, and provider experience.
Choosing a provider and regulation
Microneedling should be performed by or under the supervision of appropriately trained clinicians. Board-certified dermatologists, experienced plastic surgeons, or licensed medical aestheticians working within a medical setting are typical providers. Device regulation and clinical indications may vary; reputable professional organizations provide patient guidance and safety recommendations. For more information on dermatologic procedures and finding qualified providers, consult the American Academy of Dermatology.
Evidence and guidance
Clinical studies show microneedling can improve certain scar types and skin texture, but results depend on protocols and patient factors. Systematic reviews in dermatology journals summarize outcomes and adverse events; individual response varies. For personalized assessment, consult a licensed dermatologist or relevant specialist.
Costs and number of sessions
Costs vary by location, provider, and whether adjuncts (like PRP) are used. Multiple sessions—often spaced several weeks apart—are commonly recommended to achieve and maintain results. A realistic treatment plan should be discussed with the provider before starting.
Frequently asked questions
Is microneedling safe and effective?
Microneedling is generally considered safe when performed by a trained professional and when appropriate infection-control and aftercare measures are followed. Effectiveness varies by indication, skin type, and device; clinical studies suggest benefits for texture and some types of scarring.
How many treatments are usually needed?
Typical plans involve multiple sessions spaced several weeks apart. The number depends on treatment goals, needle depth, and how the skin responds. A provider can give a personalized estimate.
Can microneedling cause scarring or pigmentation?
While uncommon when performed correctly, scarring and post-inflammatory hyperpigmentation can occur—particularly in individuals with darker skin types or when procedures are done improperly. Proper patient selection and technique reduce risk.
Are there at-home microneedling devices, and are they recommended?
At-home devices exist with shorter needle lengths and lower injury depth, but proper training and hygiene are still essential. Overuse or improper technique can increase risk of adverse effects. Consultation with a qualified clinician is advised before attempting at-home treatments.
Who should be consulted before starting microneedling?
Consult a licensed dermatologist or qualified medical professional to evaluate suitability, discuss risks and expected outcomes, and plan appropriate pre- and post-procedure care.