Redermalization Explained: A Practical Guide to Safe Skin Rejuvenation
Get a free topical map and start building content authority today.
Redermalization is a contemporary approach to skin rejuvenation that focuses on stimulating the skin's repair and collagen remodeling processes to improve texture, firmness, and tone.
- What: Redermalization refers to treatments that restore dermal structure via collagen induction, resurfacing, or bioactive injections.
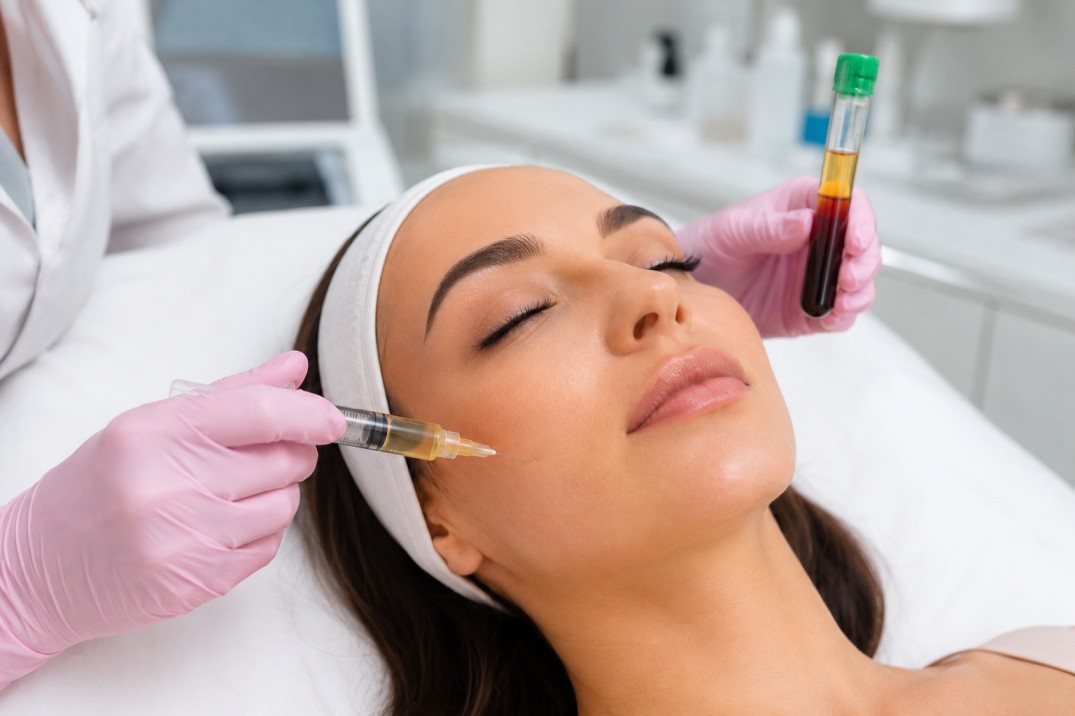
- Common methods: microneedling, platelet-rich plasma (PRP), fractional lasers, topical growth factors, and some minimally invasive injectables.
- Outcomes: improved texture, reduced fine lines, and better skin tone over weeks to months.
- Safety: select licensed providers, follow a pre/post-care checklist, and manage expectations about downtime and results.
Detected intent: Informational
What redermalization means and how it differs from other skin treatments
The term redermalization describes a set of procedures aimed at regenerating dermal structure rather than simply masking surface signs of aging. Unlike purely topical therapies or temporary fillers, redermalization techniques seek to activate collagen synthesis, remodel extracellular matrix, or replenish skin biology using mechanical, thermal, or biologic triggers. Related procedures include microneedling (collagen induction therapy), fractional laser resurfacing, and biologic adjuncts like PRP or growth-factor serums.
How redermalization works: biology and mechanisms
At the core of most redermalization approaches is controlled injury or targeted stimulation. The skin responds with inflammation, recruitment of repair cells (fibroblasts), and deposition of new collagen and elastin. Different modalities work by:
- Creating microchannels (microneedling) to trigger wound-healing pathways and increase topical absorption.
- Applying controlled thermal damage (fractional lasers, radiofrequency) to remodel collagen and tighten dermis.
- Delivering biologic signals (PRP, peptide serums) that amplify cell signaling for repair.
Common redermalization techniques and real-world examples
Microneedling and collagen induction therapy
Microneedling uses arrays of fine needles to create micro-injury. Results accumulate over several sessions and are often enhanced by topical serums or PRP applied immediately after treatment.
Fractional resurfacing
Fractional lasers and radiofrequency devices create columns of thermal injury that the surrounding tissue helps heal, reducing downtime compared with full-field resurfacing while providing measurable tightening.
Biologics and topical adjuncts
PRP (platelet-rich plasma), growth-factor-rich serums, and certain peptide formulations provide biochemical signals to expedite or amplify repair responses when used with physical stimulation.
Short example scenario
A 45-year-old patient with mild to moderate textural irregularity undergoes three microneedling sessions spaced six weeks apart, each session followed by a topical growth-factor serum. After three months, skin texture and pore appearance improve by patient-reported and clinician-measured assessments; transient redness and pinpoint bleeding resolve within a few days each session.
REPAIR Checklist: a practical framework to plan redermalization safely
- Review medical history (skin type, medications, scarring history).
- Evaluate skin goals and realistic expectations.
- Pick the right modality (microneedling, laser, PRP, or combo).
- Apply pre-treatment care (retinoid pause, sun protection, control active acne).
- Inform subject on aftercare and signs of complications.
- Review outcomes and schedule maintenance as needed.
Preparing for a redermalization treatment
Preparation reduces risk and improves outcomes. Providers commonly recommend:
- Stopping retinoids or exfoliating acids 3–7 days before treatment depending on intensity.
- Avoiding recent isotretinoin use within 6–12 months for some laser procedures; discuss systemic medications with the clinician.
- Ensuring no active infections or open wounds in the treatment area.
Aftercare, recovery, and expected timeline
Immediate effects often include redness, swelling, and sensitivity lasting from 24 hours to several days. Collagen remodeling is gradual: visible texture and firmness improvements typically emerge over 6–12 weeks and can continue for months. Use gentle cleansers, strict sun protection, and follow provider guidance on topical products during healing.
Safety, regulation, and choosing a provider
Redermalization is generally safe when performed by trained clinicians using regulated devices and sterile technique. Verify that devices are cleared or approved by relevant authorities and that the provider has documented experience. For credible guidance on dermatologic procedures and safety, consult professional resources such as the American Academy of Dermatology (AAD) for patient education and standards of care: https://www.aad.org.
Trade-offs and common mistakes
Choosing a technique involves trade-offs:
- Stronger treatments (ablative lasers) yield faster and sometimes more dramatic results but increase downtime and risk.
- Less invasive approaches (microneedling alone) have lower risk and shorter recovery but may require more sessions for comparable results.
Common mistakes include:
- Skipping a proper pre-treatment medical review (risk with isotretinoin or bleeding disorders).
- Using unregulated products or non-sterile PRP preparation.
- Expecting immediate, permanent results—redermalization often needs maintenance.
Practical tips for better outcomes
- Follow the REPAIR checklist before any procedure to minimize preventable complications.
- Choose a staged plan (start conservative and escalate if needed) rather than an aggressive one-off approach.
- Prioritize sun protection daily—UV exposure undermines collagen remodeling and accelerates relapse.
- Maintain realistic expectations: measure success by texture and quality improvements, not dramatic wrinkle erasure in a single session.
Core cluster questions for further reading
- How many sessions of redermalization are typically needed for visible results?
- What are the differences between microneedling and fractional laser treatments?
- When is PRP a useful adjunct to physical redermalization methods?
- How should skin be prepared and protected before and after redermalization?
- What are realistic outcome timelines and signs that a complication is developing?
Who benefits most from redermalization
Good candidates typically have mild to moderate photoaging, texture irregularities, or early laxity and realistic expectations. People with active inflammatory skin disease, certain bleeding disorders, or recent isotretinoin use need individualized assessment. For complex conditions, referral to a board-certified dermatologist or plastic surgeon can clarify options.
Measuring success: practical metrics
Trackable outcomes include clinical photographs under consistent lighting, validated skin texture scales, patient-reported improvement scores, and objective measures like skin elasticity devices where available. Documenting progression across sessions helps decide whether to continue, switch modality, or add maintenance treatments.
Summary and next steps
Redermalization is a versatile approach to skin rejuvenation that emphasizes dermal repair rather than temporary camouflage. Use the REPAIR checklist to plan care, choose licensed providers and regulated devices, and set realistic timelines for gradual improvement. Integrating sensible pre/post-care and ongoing sun protection maximizes durability.
FAQ: What is redermalization and is it right for my skin?
Redermalization encompasses treatments aimed at stimulating new collagen and remodeling the dermis; suitability depends on skin concerns, medical history, and risk tolerance. A clinician assessment will determine the most appropriate modality.
FAQ: How long until redermalization produces visible results?
Visible improvements usually begin at 6–12 weeks as collagen remodels, with progressive gains over several months. Multiple sessions spaced weeks apart are common.
FAQ: Are there risks with redermalization treatments?
Risks include temporary redness, infection, pigment changes, and scarring in uncommon cases. Risk is reduced by provider training, sterile technique, and following pre/post-care instructions.
FAQ: Can redermalization be combined with other skin rejuvenation methods?
Yes. Combinations—such as microneedling with PRP or alternating laser and microneedling—can enhance results but require careful planning to manage downtime and healing.
FAQ: How should skin be cared for after a redermalization session?
Aftercare typically includes gentle cleansing, avoiding active exfoliants until healed, daily broad-spectrum sunscreen, and following any topical or oral medications prescribed by the clinician to reduce inflammation or infection risk.