Everything to Know About Sleeping Pills: Types, Risks, and Safer Alternatives
👉 Best IPTV Services 2026 – 10,000+ Channels, 4K Quality – Start Free Trial Now
Introduction to sleeping pills
Sleeping pills are medications used to help people fall asleep, stay asleep, or both. They include prescription drugs and over-the-counter options that act on brain chemistry, helping to reduce the time it takes to fall asleep or increasing total sleep time. This guide summarizes common types, how they work, potential risks, and nonpharmacological alternatives to support informed discussions with licensed clinicians.
- Sleeping pills span multiple drug classes with different mechanisms and durations.
- Benefits may include faster sleep onset or longer sleep, but risks include daytime drowsiness, dependence, and interactions.
- Short-term use is common; long-term safety varies by medication and individual factors.
- Behavioral approaches, sleep hygiene, and targeted therapies are alternatives recommended by sleep specialists.
How sleeping pills work
Different sleeping pills target brain systems that regulate arousal and sleep. Common mechanisms involve enhancing the activity of gamma-aminobutyric acid (GABA), a neurotransmitter that reduces neural activity, or modulating melatonin receptors involved in circadian timing. Effects vary by onset speed, duration, and whether the drug mostly affects sleep initiation or maintenance.
Types of medications commonly called sleeping pills
Medications used as sleeping pills fall into several categories. Each class has typical uses and characteristic effects:
- Nonbenzodiazepine sedative-hypnotics: Often prescribed for short-term insomnia; generally act on GABA receptors and are designed to have fewer muscle-relaxant or anticonvulsant effects than older benzodiazepines.
- Benzodiazepines: Older sedative drugs that can be effective for insomnia but carry higher risks of tolerance and dependence with prolonged use.
- Melatonin receptor agonists: Mimic or enhance melatonin signaling to help regulate sleep–wake timing; often used for circadian-related sleep problems.
- Orexin receptor antagonists: Work by blocking wake-promoting orexin pathways and can help with both sleep onset and maintenance.
- Antidepressants and antihistamines: Some agents with sedating properties are used off-label for sleep, especially when other symptoms like mood disturbance are present; over-the-counter antihistamines can cause drowsiness but may have next-day effects.
Potential risks and common side effects
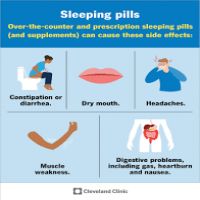
Side effects depend on the medication but commonly include daytime sleepiness, dizziness, memory or coordination problems, and complex sleep-related behaviors (for example, sleepwalking). Longer-term concerns can include tolerance, dependence, rebound insomnia after stopping, and interactions with alcohol or other central nervous system depressants. Older adults are more vulnerable to falls and cognitive effects.
Regulation, prescribing practices, and monitoring
Regulatory agencies and professional bodies provide guidance on safe prescribing and monitoring. For drug-specific safety information and updates, consult regulatory resources such as the U.S. Food and Drug Administration (FDA). Healthcare providers typically weigh the severity and duration of insomnia, underlying causes, patient age, comorbidities, and potential drug interactions before recommending a sleeping pill.
U.S. Food and Drug Administration
Who may need to avoid sleeping pills
Certain groups require extra caution, including older adults, people with a history of substance use disorder, those with severe respiratory disease, and individuals taking medications that interact with sedatives. Sleep specialists and pharmacists can help assess risks based on medical history and current therapy.
Safer use and monitoring considerations
- Use the lowest effective dose for the shortest duration appropriate to the clinical situation.
- Inform prescribing clinicians about all medications, supplements, and alcohol use to reduce interaction risks.
- Be aware of activities that require alertness the next day, such as driving or operating machinery.
- Regularly reassess the need for ongoing treatment and monitor for tolerance or adverse effects.
Non-drug alternatives and complementary approaches
Evidence-based nonpharmacological treatments can address chronic insomnia and may reduce reliance on sleeping pills. Cognitive behavioral therapy for insomnia (CBT-I) is recommended by sleep medicine organizations and has been shown in clinical studies to improve sleep over the long term. Other supportive measures include consistent sleep schedules, controlling light and noise, limiting stimulating activities before bedtime, and addressing sleep-disrupting conditions such as sleep apnea or restless legs syndrome.
When to seek more help
Persistent sleep problems that affect daytime functioning or quality of life warrant evaluation by a licensed clinician or a sleep specialist. Underlying medical, psychiatric, or sleep disorders may need targeted treatment. For serious symptoms like severe daytime sleepiness, episodes of stopped breathing during sleep, or sudden changes in behavior, prompt professional evaluation is important.
Frequently asked questions
Are sleeping pills safe for long-term use?
Safety for long-term use depends on the specific medication, the person's health status, and monitoring practices. Many clinicians prefer short-term use or intermittent therapy; some drugs have more supporting data for longer-term treatment under supervision. Regulatory agencies and clinical guidelines recommend individualized assessment and periodic reevaluation.
What are common side effects of sleeping pills?
Common side effects include daytime drowsiness, dizziness, impaired coordination, and problems with memory or concentration. Some medications can cause complex sleep behaviors or breathing problems in susceptible individuals.
Can sleeping pills interact with other medications or alcohol?
Yes. Sleeping pills can interact with other central nervous system depressants, certain antidepressants, and medications that affect liver enzymes. Alcohol can increase sedation and risk. A pharmacist or prescribing clinician can review potential interactions.
Are there effective alternatives to sleeping pills?
Behavioral treatments such as cognitive behavioral therapy for insomnia (CBT-I), improved sleep hygiene, and treatment of underlying medical or psychiatric conditions are effective alternatives and are recommended by sleep specialists for many people with chronic insomnia.
How quickly do sleeping pills work and how long do effects last?
Onset and duration vary by medication. Some agents act within 15–30 minutes and wear off within a few hours; others are formulated for longer action to reduce night awakenings. Medication choice often depends on whether difficulty is falling asleep, staying asleep, or both.
Can anyone safely take over-the-counter sleeping aids?
Over-the-counter options are widely available but are not risk-free. Older adults and people with certain medical conditions may be at higher risk of adverse effects. Professional assessment helps determine whether an over-the-counter product is appropriate.
How to learn more or get personalized guidance?
Clinical guidance from licensed clinicians and published recommendations from organizations such as the American Academy of Sleep Medicine, the Centers for Disease Control and Prevention (CDC), and peer-reviewed medical literature provide sources for further information. Healthcare professionals can offer individualized assessment and monitoring plans.